That dull, throbbing ache at the very back of your mouth is unmistakable. Wisdom tooth pain has a way of dominating your entire focus, making it hard to eat, sleep, or think about anything else. You're not just imagining it—it's a real, often complex dental issue that millions of adults face. The immediate question is always the same: what can I do right now, and is this serious enough to call the dentist? Let's cut through the noise. This guide will walk you through exactly why it hurts, how to manage the discomfort safely at home, and the non-negotiable signs that you need professional help, potentially for a wisdom tooth removal.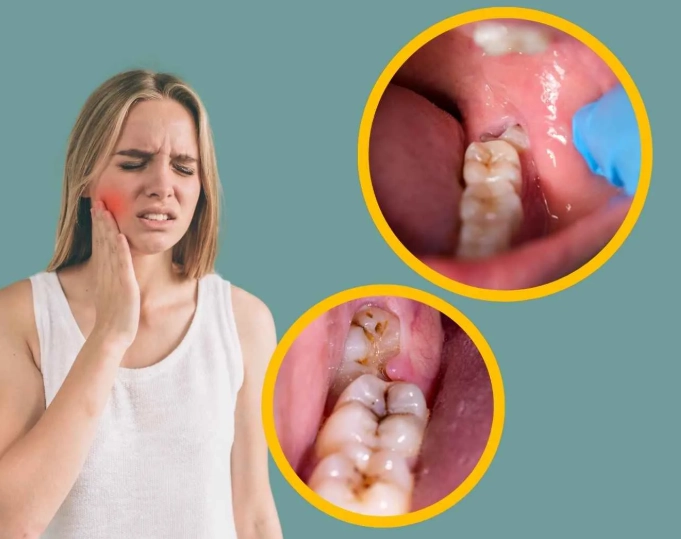
What's Inside This Guide
What Exactly Causes Wisdom Tooth Pain?
It's not just "teeth coming in." The pain originates from a fundamental mismatch: our jaws have evolved to be smaller, but we still grow the same number of teeth. Your third molars, the wisdom teeth, are the last to erupt, usually between ages 17 and 25. By then, there's often no room left.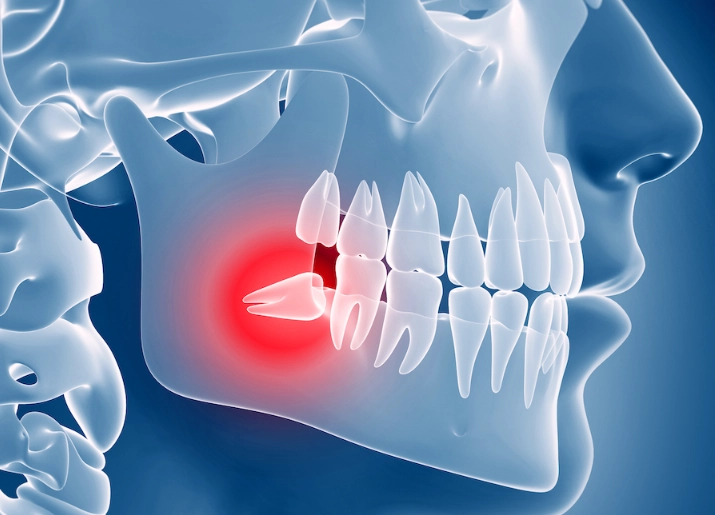
This space crunch leads to several specific, painful scenarios:
The Problem of Impaction
An impacted wisdom tooth is one that fails to fully emerge through the gums. It gets stuck. This is the core issue for most severe pain cases. The type of impaction dictates the kind of trouble you'll have.
| Type of Impaction | What It Means | Common Pain & Risks |
|---|---|---|
| Mesioangular | Tooth is angled forward, towards the front of the mouth. | Most common type. Presses hard against the molar in front, causing crowding, decay in both teeth, and gum pain. |
| Vertical | Tooth is straight but trapped beneath the gum line. | May partially erupt, creating a gum flap (operculum) that traps food and leads to infection (pericoronitis). |
| Horizontal | Tooth lies completely on its side, growing into the roots of the adjacent molar. | Often the most damaging. Can destroy the roots of the healthy second molar, causing severe, constant pain. |
| Distoangular | Tooth is angled backward, towards the rear of the jaw. | Less common, but can cause jaw pain and issues with the jaw joint (TMJ). |
I've seen patients who thought they had an earache or sinus pressure for weeks, only to find out it was a horizontally impacted wisdom tooth. The pain can radiate in surprising ways.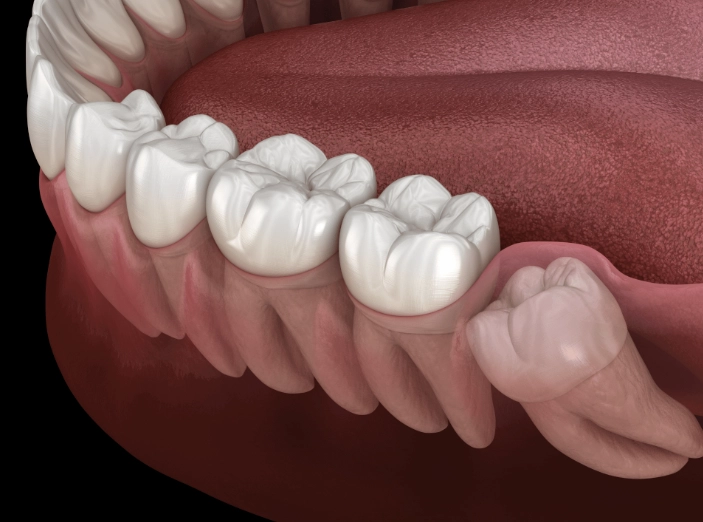
Pericoronitis: The Infection You Can Feel
This is a big one. When a wisdom tooth partially erupts, a flap of gum tissue often remains over it. This flap is a perfect trap for food particles and bacteria. The resulting infection—pericoronitis—causes intense, localized pain, swelling, a bad taste, and sometimes difficulty opening your mouth. It's a clear signal that the area is no longer manageable with brushing alone.
Crowding and Decay
Even if a wisdom tooth manages to come in fully, it's often so far back and angled so awkwardly that it's impossible to clean properly. Plaque builds up rapidly, leading to cavities in the wisdom tooth itself and the precious molar in front of it. The pain from this decay can be sharp and sensitive to temperature or sweets.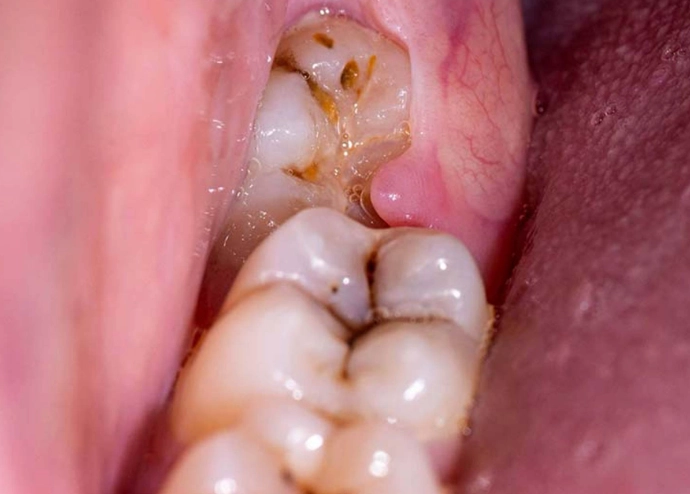
How to Get Wisdom Tooth Pain Relief at Home (Safely)
It's 10 PM, your dentist's office is closed, and the throbbing is getting worse. Here are steps you can take that actually work. Think of these as temporary measures to bridge the gap until you see a professional.
Salt Water Rinse: This isn't just old advice; it's effective. Mix half a teaspoon of salt in a glass of warm water. Swish gently for 30 seconds, focusing on the back of your mouth. Do this 2-3 times a day, especially after eating. The salt helps reduce inflammation, draws out minor infection, and soothes irritated gums.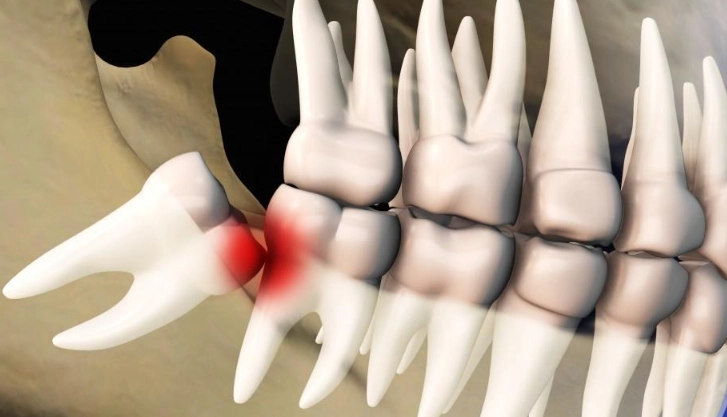
Cold Compress: Hold an ice pack or a bag of frozen peas wrapped in a thin cloth against your cheek, over the painful area. Do this for 15 minutes on, 15 minutes off. It constricts blood vessels, reducing swelling and numbing the pain. Don't apply heat to an unexplained toothache—if there's an infection, heat can make it spread.
Over-the-Counter Pain Relievers: Ibuprofen (Advil, Motrin) is typically more effective for dental pain than acetaminophen (Tylenol) because it tackles both pain and inflammation. Follow the package directions. A common dental dosing strategy is to alternate ibuprofen and acetaminophen, but check with your pharmacist or doctor first to ensure it's safe for you.
Keep It Clean (Gently): Try to brush carefully around the area. Using a soft-bristled toothbrush and an antiseptic mouthwash without alcohol can help reduce bacterial load. If there's a gum flap, you can try gently flushing underneath it with a dental irrigator on the lowest setting or a curved-tip syringe.
What NOT to do: Never place aspirin or any other painkiller directly against your gum. It will burn your gum tissue, creating a painful ulcer on top of your toothache. Also, avoid poking the area with toothpicks or sharp objects.
When Wisdom Tooth Pain Means You Must See a Dentist
Home care has its limits. These symptoms are red flags that the problem is beyond a simple rinse or painkiller. Delaying can lead to serious complications.
You should call a dentist or oral surgeon if you experience:
Fever: This is your body signaling a systemic infection.
Swelling that spreads: If swelling extends to your cheek, jawline, or under your tongue, the infection is moving into the deeper spaces of your head and neck. This is called a cellulitis and is a medical emergency.
Difficulty swallowing or breathing: An immediate emergency. Swelling in these areas can obstruct your airway.
Pus discharge from around the tooth.
Trismus (Lockjaw): Inability to open your mouth more than a finger's width.
Severe, unrelenting pain that isn't touched by over-the-counter medication.
Pain that lasts more than 2-3 days without improvement.
In these cases, the goal isn't just pain relief; it's to control the infection, often with antibiotics, before any extraction can be safely performed.
What to Expect from Wisdom Tooth Extraction & Recovery
If your dentist recommends removal, it's usually for a very good reason—to solve the current pain and prevent future, more complex issues. The procedure itself is done under local anesthesia, sedation, or general anesthesia, so you won't feel pain during it.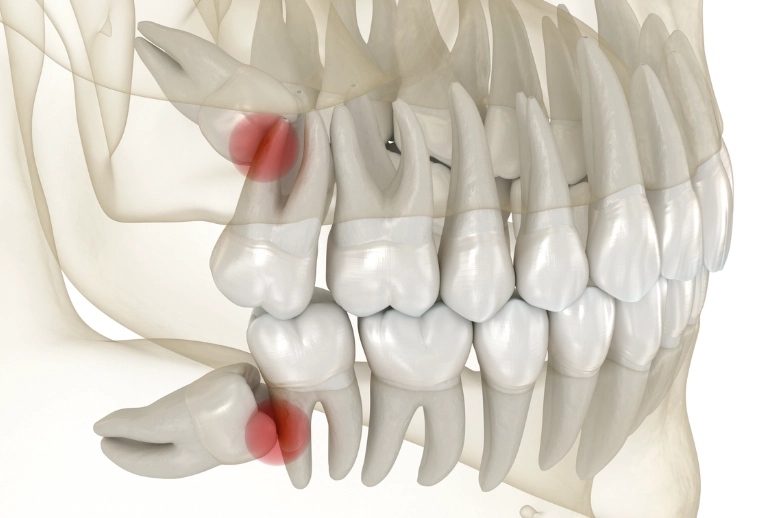
The recovery timeline is where realistic expectations matter:
First 24 Hours: Bleeding is normal. Bite firmly on the gauze pads. Swelling peaks around day 2-3. Stick to cool, soft foods (yogurt, pudding, smoothies). Use ice packs. Absolutely no sucking through straws, spitting, or smoking—these can dislodge the crucial blood clot and cause a dry socket, which is intensely painful.
Days 2-4: Swelling and stiffness are most pronounced. Transition to lukewarm, soft foods (mashed potatoes, scrambled eggs). Begin very gentle saltwater rinses after 24 hours. Pain should be manageable with prescribed or OTC meds.
Week 1: Swelling subsides. Stitches may dissolve or need removal. You can gradually reintroduce more solid foods as comfort allows, but avoid crunchy or chewy foods on the surgical side.
Full healing of the bone and gum tissue underneath takes several months, but most people feel back to normal activities within a week.
Your Wisdom Tooth Pain Questions, Answered
Can wisdom tooth pain go away on its own?
The acute flare-up from pericoronitis (gum flap infection) might temporarily subside with improved hygiene or a course of antibiotics, but the underlying problem—the poorly positioned tooth—remains. It's like quieting a smoke alarm instead of putting out the fire. The pain will almost certainly return, often worse, because the tooth continues to be a magnet for food and bacteria.
How painful is wisdom tooth removal? Is it as bad as people say?
The procedure itself isn't painful due to anesthesia. The recovery involves discomfort, but modern pain management protocols make it very manageable. The horror stories often come from two places: trying to do too much too soon (like eating chips on day 3), or developing a dry socket from smoking or using a straw. Follow your surgeon's aftercare instructions to the letter, and your experience will be vastly more positive.
My wisdom teeth came in straight and don't hurt. Do I still need to remove them?
This is a common point of debate. The American Association of Oral and Maxillofacial Surgeons states that even symptom-free wisdom teeth can be problematic. The challenge is cleaning them. If you can consistently floss and brush all surfaces perfectly, and your dentist confirms they are fully erupted with healthy gums, you might keep them. But most people can't clean them effectively, leading to silent decay and gum disease that only shows up years later. Proactive removal is often the simpler, safer long-term choice.
What's the one thing most people get wrong about managing wisdom tooth pain at home?
They treat it like a headache—just pop a pill and wait. Dental pain is almost always a structural or infectious problem. Relying solely on painkillers masks the symptoms while the actual damage (decay, gum destruction, bone loss) continues unchecked. Pain relief is step one, but diagnosing and fixing the cause with a dental professional is the non-negotiable step two.
Wisdom tooth pain is your body's unmistakable alert system. Listen to it. Temporary relief is possible, but a lasting solution requires understanding the "why" behind the ache and taking decisive action with a qualified dentist or oral surgeon. Don't let fear of the procedure condemn you to years of recurring pain and bigger dental problems.