Let’s cut to the chase. For years, the story has been simple: your wisdom teeth come in, they push all your other teeth forward, and suddenly your beautifully straight smile turns into a crowded mess. It’s a narrative so common it feels like fact. Dentists often recommend preemptive removal to “protect your orthodontic work.” But after seeing hundreds of cases and diving into the actual research, I think this standard line oversimplifies a much more interesting – and sometimes controversial – story.
The real link between wisdom teeth and dental crowding is nuanced. Sometimes they’re a contributing factor; often, they’re just an easy scapegoat for shifts that have more complex causes. This guide will walk you through what actually happens in your jaw, when you should be concerned, and what your treatment options really look like beyond the standard “just yank ‘em out” advice.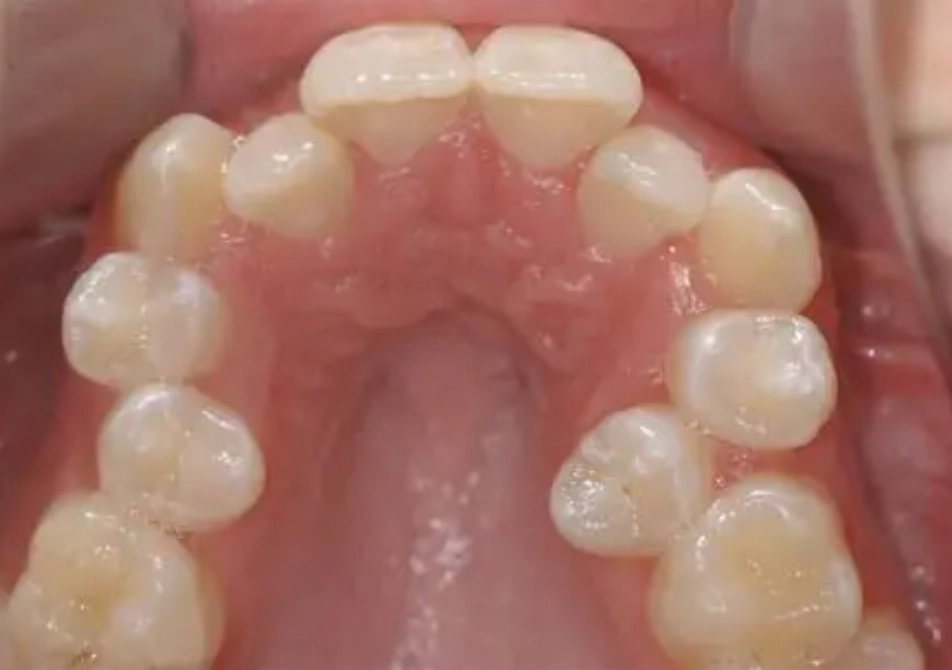
What’s Inside?
The Real Relationship: Do Wisdom Teeth Actually Cause Crowding?
Here’s the non-consensus view I’ve formed after years in practice: wisdom teeth are rarely the primary driver of significant dental crowding. They’re more like the final passenger trying to squeeze onto an already full bus.
The American Association of Orthodontists states that the most significant cause of crowding is a mismatch between jaw size and tooth size – you simply inherited a jaw that’s a bit too small for all 32 teeth. Crowding in your late teens and twenties is often just the continuation of a natural, lifelong process called “late mandibular growth rotation” and “mesial drift” (teeth naturally tend to shift forward over time). Your wisdom teeth, erupting between ages 17 and 25, just happen to show up right when you might be noticing these subtle shifts.
Think of it this way. If your teeth have plenty of space, an erupting wisdom tooth has room to come in straight. No problem. But if your dental arch is already tight – maybe your lower jaw is a little narrow – that wisdom tooth has nowhere to go. It might become impacted (stuck), come in sideways, or indeed, exert pressure on the tooth in front of it. This pressure can contribute to crowding, but it’s usually amplifying an existing space issue, not creating one from scratch.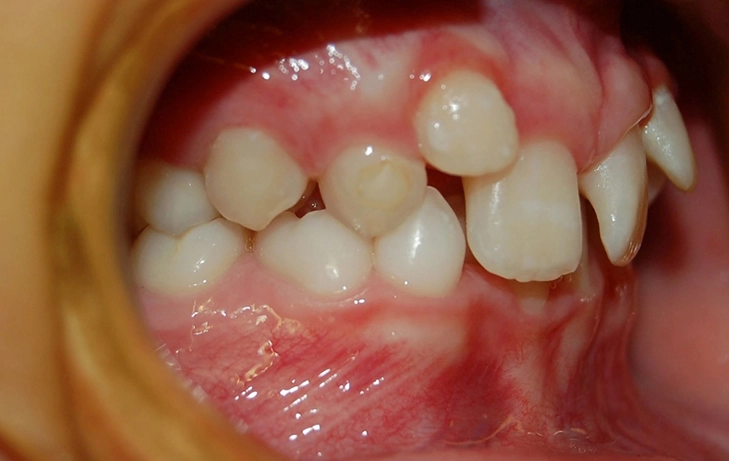
Signs Your Wisdom Teeth Might Be a Problem
So when should you suspect your wisdom teeth are part of the crowding equation? Look for these specific signs, especially if you’ve had braces before:
Localized Crowding at the Back: You notice the very back teeth, particularly your second molars, starting to tilt or rotate. This is more telling than general front-tooth crowding.
Recurrence After Braces: Your lower front teeth, which were perfectly straight after orthodontics, are gradually overlapping again. While wisdom teeth can be a factor, research published in the American Journal of Orthodontics and Dentofacial Orthopedics suggests the primary culprit is often not wearing your retainer as directed. Still, impacted wisdom teeth can add to the pressure.
Pain or Pressure Sensation: A dull ache or feeling of pressure in the very back of your jaw, coinciding with visible tooth movement.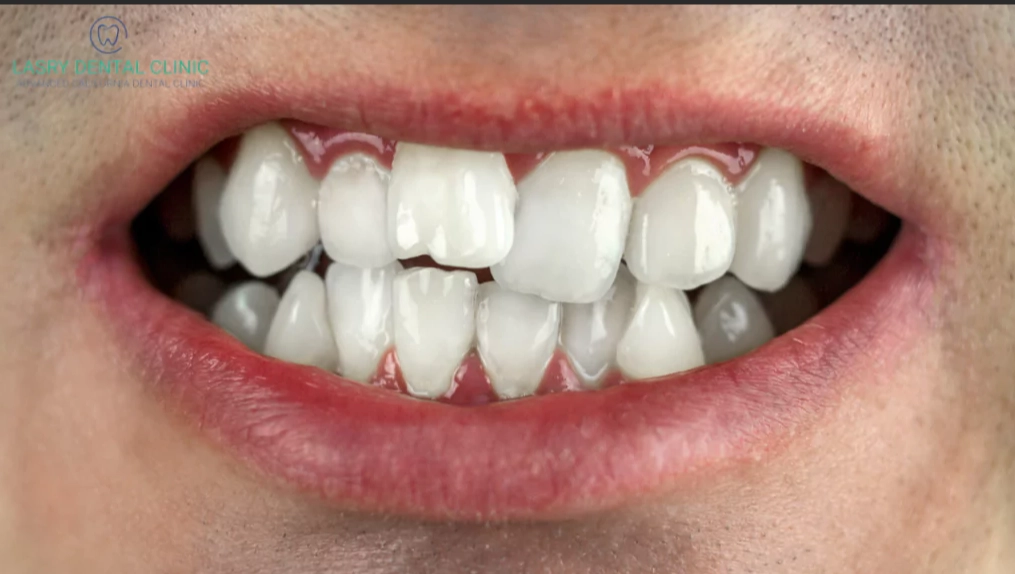
Beyond the X-Ray: How to Get a Proper Diagnosis
If you’re worried about crowding, getting a panoramic X-ray (OPG) is step one. It shows the position, angle, and root formation of all your wisdom teeth. But that’s just the start. A proper assessment needs context.
An orthodontist will look at your dental casts or digital scans to measure arch length and tooth size. They’ll check your occlusion (how your teeth bite together). They’ll also consider your age and whether you’ve had previous orthodontic treatment. The goal is to answer: Is there actually enough space for these teeth to erupt functionally?
I’ve seen too many patients come in with a referral for wisdom teeth extraction based solely on a crowded lower incisor and a panoramic film showing teeth angled slightly forward. Sometimes, the best course is active monitoring. If the teeth are fully impacted in bone, not causing decay on the adjacent tooth, and not associated with a cyst, the risks of surgery might outweigh the potential benefits for preventing crowding.
At the Treatment Crossroads: Removal vs. Monitoring
This is the big decision. Let’s break down the scenarios where removal is typically recommended versus where you might have other options.
| Scenario | Typical Recommendation | Reasoning & Nuances |
|---|---|---|
| Active, Symptomatic Impaction (Pain, infection, cyst formation) |
Extraction | This is clear-cut. The tooth is causing pathology. Removal resolves the immediate problem and eliminates a future source of pressure. |
| Severe Lack of Space & Existing Crowding (Teeth are visibly crooked, X-ray shows teeth horizontal or severely angled) |
Extraction (often combined with orthodontics) | Removing the wisdom teeth creates a bit of space at the back and removes a potential force. However, it will not straighten already crooked teeth by itself. Orthodontics (braces/aligners) is still needed. |
| Post-Orthodontic Prevention (Braces just came off, wisdom teeth are still under the gums) |
Often Extraction, but Debate Exists | The classic “preventive” reason. The logic is to remove a potential force for relapse. Some studies, like those cited by the AAO, support this. Others show minimal effect if retainers are worn diligently. A long-term retainer plan is arguably more critical. |
| Asymptomatic, Full Bony Impaction in an Older Adult (Over 30, no history of cysts, no decay on adjacent tooth) |
Often Monitoring | The risks of surgery (nerve injury, prolonged healing) increase with age. If it’s not causing problems and is fully encased in bone, the “if it ain’t broke” principle can apply. Regular X-rays every few years to check for changes are key. |
The cost factor is real. A straightforward extraction might cost $300-$600 per tooth, while impacted surgical removal can range from $600 to $1500 per tooth. Insurance often covers a portion if deemed “medically necessary” (e.g., due to impaction or infection), but less so for purely “orthodontic/preventive” reasons.
The Recovery Reality: What They Don’t Put on the Pamphlet
If you do opt for removal, here’s the unfiltered timeline and tips you won’t always get from the standard post-op sheet. I’ve had mine out, and I’ve guided hundreds through it.
Days 1-3 (The Swelling Zone): This is the hardest part. Your face will swell, peaking around day 2 or 3. It looks worse than it feels for most. Ice packs are your best friend – 20 minutes on, 20 minutes off. Stick to a strict schedule, even while sleeping. The pain is manageable with prescribed meds, but the real discomfort is the stiffness and the inability to open wide. Liquid and soft foods only. Pro tip: Protein shakes, blended soups (not hot!), and Greek yogurt will be more satisfying than just apple sauce.
Days 4-7 (The Turning Point): Swelling starts to subside. Bruising might appear – yellow and green around the jawline – which is normal. You can gradually introduce mashed potatoes, scrambled eggs, very soft pasta. The most critical mistake here? Thinking you’re healed and using a straw or smoking. The suction can dislodge the blood clot, leading to a painful “dry socket.” Just don’t do it.
Week 2 Onward (The Slow Grind): You’ll feel mostly normal, but the extraction sites will have deep holes that slowly fill in with tissue over 4-6 weeks. You’ll need to gently irrigate these holes with a syringe after eating to keep them clean. Chewing at the very back will feel weird for a while. Full bone remodeling takes months.
This matters for the crowding discussion because a smooth recovery means less overall stress on your system and a quicker return to normal oral hygiene, which is essential for maintaining the health of your now-more-vulnerable adjacent teeth.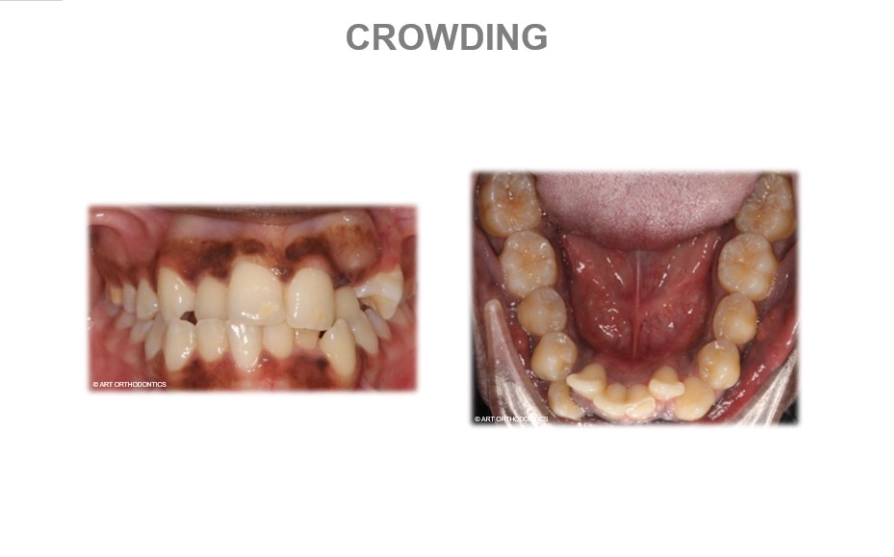
Your Top Wisdom Teeth & Crowding Questions, Answered
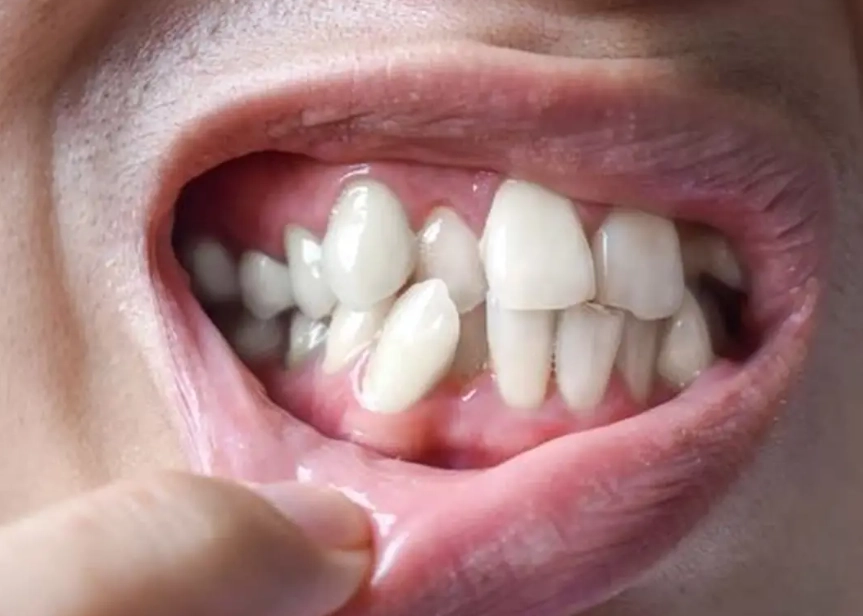 My orthodontist says I need braces and must remove all four wisdom teeth first. Is this always mandatory?
My orthodontist says I need braces and must remove all four wisdom teeth first. Is this always mandatory?