That nagging toothache you've been ignoring, or that weird sensitivity to hot coffee—could it be something serious? As someone who's worked in dental health for over a decade, I've seen countless patients who wish they'd paid attention to the subtle hints their teeth were giving them. Needing a root canal doesn't always start with a dramatic, unbearable pain. More often, it begins with whispers. Ignoring these whispers is where people get into real trouble, leading to more complex procedures or even tooth loss. Let's cut through the anxiety and talk plainly about the first signs that the nerve inside your tooth might be in trouble.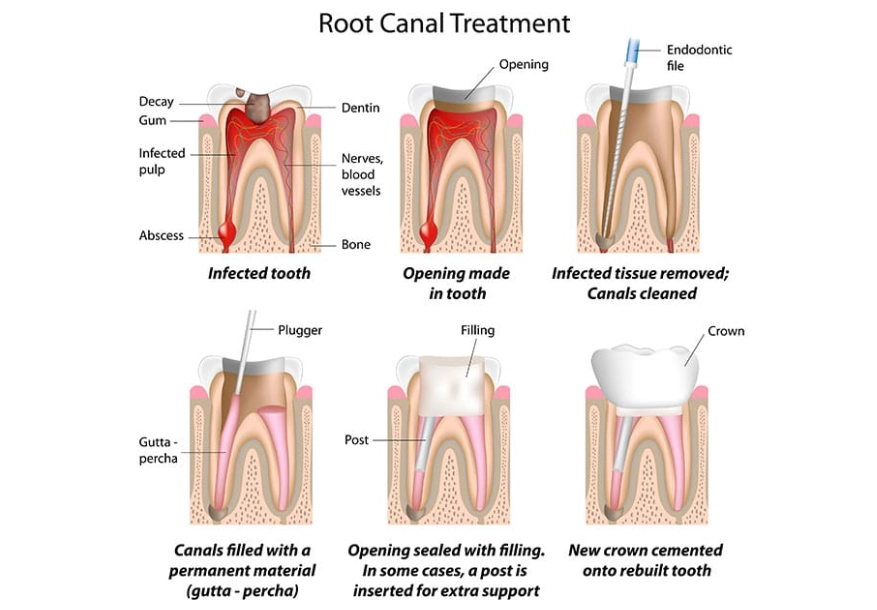
What You’ll Find in This Guide
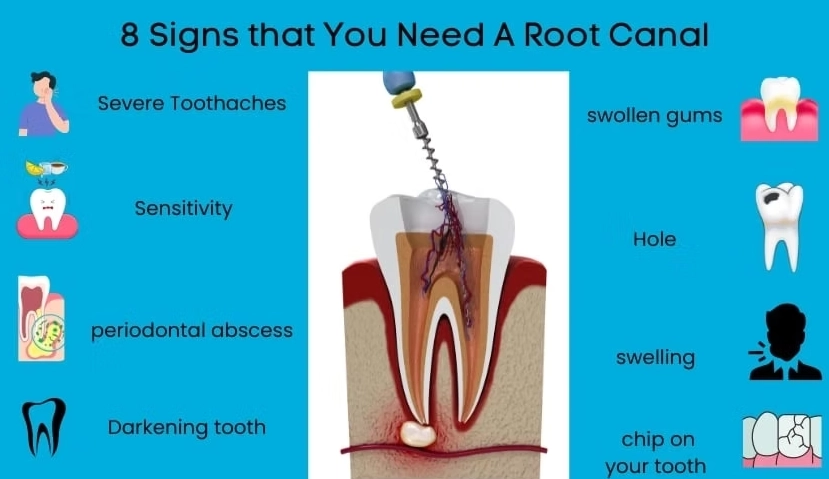
The Top 5 Early Signs You Should Never Ignore
Think of these as your tooth's distress signals. One alone might be a fluke. Two or more? It's time to call your dentist.
1. Persistent Toothache This isn't your typical "sugar ache" that fades in seconds. We're talking about a deep, dull ache that lingers for minutes or even hours. It might throb, especially when you lie down (increased blood pressure to the head can amplify the pain). A classic red flag is pain that wakes you up at night. I had a patient who thought it was sinus pressure for weeks because the ache seemed to come from several upper teeth. Turns out, it was one molar with a dying nerve referring pain across a wider area.
2. Sensitivity to Hot and Cold That Lingers Everyone gets a zing from ice cream. The key difference here is duration. With a healthy tooth, the sharp sensation stops the moment the stimulus is gone. If you sip hot tea and the pain or sensitivity continues for 10, 20, or 30 seconds after you've swallowed, that's a major warning sign. It often means the nerve is damaged and can't recover normally. Cold sensitivity that lingers is a particularly strong indicator of irreversible pulpitis—the fancy term for a nerve that's past the point of healing on its own.
3. Pain When You Bite or Apply Pressure You chew your food and feel a sharp pain in one specific tooth. Or maybe you tap on it with your fingernail and it feels tender. This often signals that the infection from the inner tooth has spread to the ligaments and bone surrounding the root tip. The area becomes inflamed, and pressure causes pain. Sometimes, patients tell me the tooth even feels "taller" than the others because it's slightly pushed out of its socket by the swelling.
4. A Pimple on Your Gums This one surprises people. It's not a typical pimple. Dentists call it a fistula or a gum boil. It's a small, pimple-like bump on the gums near the root of the problematic tooth. It might drain a bad-tasting fluid (pus) and then shrink, only to come back later. This is your body's attempt to create a drainage pathway for the infection brewing at the root's end. It's a clear sign the problem has been there for a while. Seeing this means you've moved past "early" signs into a more advanced stage that needs immediate attention.
5. Darkening or Discoloration of the Tooth A single tooth turning gray, dark yellow, or brownish can indicate that the nerve inside has died. The breakdown of internal tissue releases pigments that stain the tooth from the inside out. This often happens after a significant trauma to the tooth, even if it was years ago. You might not feel any pain at this stage because the nerve is dead, but the infection is still active at the root tip. This is a silent but serious sign.
Why Do These Signs Mean You Might Need a Root Canal?
A root canal becomes necessary when the soft tissue inside your tooth (the pulp) becomes inflamed or infected. This pulp contains nerves, blood vessels, and connective tissue. Once this damage is severe or irreversible, the pulp can't heal itself. The goal of the root canal procedure is to remove this diseased tissue, clean and disinfect the inner chambers of the tooth, and then seal it to prevent re-infection. It's not about removing the roots of your tooth; it's about removing the tissue inside the roots.
The American Association of Endodontists (AAE) explains that deep decay, repeated dental procedures on a tooth, a crack or chip in the tooth, or trauma can all lead to pulp damage. The signs listed above are your body's response to that damage—pain from inflammation, sensitivity from nerve irritation, and a gum pimple from the immune system fighting an infection at the root's tip.
The Big Misconception: It’s Not Always About Pain
Here's the insider perspective many general articles miss: the absence of pain does not mean the absence of a problem. I've diagnosed many needed root canals on teeth that weren't actively hurting the patient. A dead nerve (necrosis) may not send pain signals, but the bacteria and their byproducts are still leaking out the end of the root, causing a chronic infection in the jawbone. This can show up only on an X-ray as a dark shadow around the root tip, called a periapical radiolucency. That's why regular dental check-ups with X-rays are non-negotiable. They catch what you can't feel.
When It Becomes an Emergency: If any mild sign suddenly escalates to severe, throbbing pain, significant facial swelling, fever, or a foul taste in your mouth that won't go away, you're likely dealing with an acute abscess. This is a dental emergency. Don't wait for an appointment next week. Contact your dentist or an emergency dental clinic immediately.
What to Do If You Notice Any of These Signs
Panicking won't help. Taking systematic action will.
First, schedule a dental appointment. Be specific when you call. Tell them, "I have a persistent toothache and lingering sensitivity to hot and cold in one tooth." This helps them prioritize your visit. Don't just say "I have a toothache."
Second, manage discomfort until your appointment. Over-the-counter anti-inflammatories like ibuprofen can help reduce inflammation and pain. Avoid chewing on that side of your mouth. Stick to softer foods. You can try a cold compress on the outside of your cheek for 15-minute intervals to numb the area.
Third, understand the diagnosis process. Your dentist isn't going to jump straight to "root canal." They will: 1. Review your symptoms and dental history. 2. Perform clinical tests: tapping on teeth (percussion), checking for gum swelling, and applying hot/cold stimuli to pinpoint the problem tooth. 3. Take a dental X-ray. This is crucial. It shows the condition of the bone around the roots and can reveal hidden decay or infection areas that aren't causing symptoms yet.
Based on this combination of tests, they'll determine if the pulp damage is reversible (possibly treated with a large filling or crown) or irreversible (requiring a root canal). Sometimes, the diagnosis isn't black and white, and your dentist may recommend a "wait and see" approach with a medicated filling, but they'll be very clear about what signs mean it's failing.
Your Root Canal Questions, Answered
If my tooth stops hurting on its own, does that mean the problem is gone?
This is one of the most dangerous assumptions. Often, a toothache stops because the nerve has finally died. The pain-generating tissue is gone, but the bacterial infection at the root tip is very much alive and can spread silently into your jawbone. The problem hasn't gone away; it's just entered a new, potentially more destructive phase.
Can a tooth that needs a root canal heal itself without treatment?
No. Once the dental pulp is severely infected or necrotic (dead), it cannot regenerate or heal. Your body might wall off the infection with a chronic abscess (that gum pimple), but it's a stalemate, not a cure. The source of the infection remains inside your tooth and will eventually cause another flare-up or bone loss.
My dentist says I need a root canal, but I'm only feeling mild sensitivity. Should I get a second opinion?
It's always your right to seek a second opinion, especially for a significant procedure. Consider seeing an endodontist, a dentist who specializes in root canals. They have advanced training and imaging tools like cone-beam CT scans. Often, their diagnosis confirms the general dentist's. The key is to base the decision on objective evidence—the X-ray and clinical tests—not just the level of pain you feel. Mild symptoms with clear radiographic evidence of infection absolutely warrant treatment.
Is it better to just pull the tooth instead of getting a root canal?
Almost never as a first choice. Saving your natural tooth with a root canal and a crown is almost always the better long-term strategy for your oral health. It maintains your bite, prevents neighboring teeth from shifting, and preserves jawbone. An extraction might seem cheaper and faster, but replacing that tooth with an implant or bridge is more costly and invasive. The
American Association of Endodontists strongly advocates for saving natural teeth whenever possible.
How long can I safely wait if I suspect I need a root canal?
There is no safe waiting period. You're gambling with your health. A localized infection can turn into a spreading cellulitis or a serious systemic issue. At the very least, delay allows the infection to destroy more supporting bone, which can compromise the long-term success of the root canal or even make saving the tooth impossible. Call your dentist within days, not weeks, of noticing persistent symptoms.





