You just had a root canal. The pain is gone, and you're relieved. But then, a few weeks or months later, you catch a glimpse of that tooth in the mirror. It looks... off. Maybe it's a little darker than its neighbors. Maybe it has a slight grey or yellowish tint. Your heart sinks. Did the procedure fail? Is this normal? Will your smile ever look the same again?
Let's cut to the chase: Yes, a tooth can look different after a root canal. It's one of the most common, yet least discussed, side effects of the procedure. But here's the crucial part you need to know: It doesn't have to be permanent, and it's often preventable or fixable. I've seen this scenario countless times in my practice. The anxiety it causes is real, but so are the solutions. This isn't just about aesthetics; it's about feeling confident in your smile again.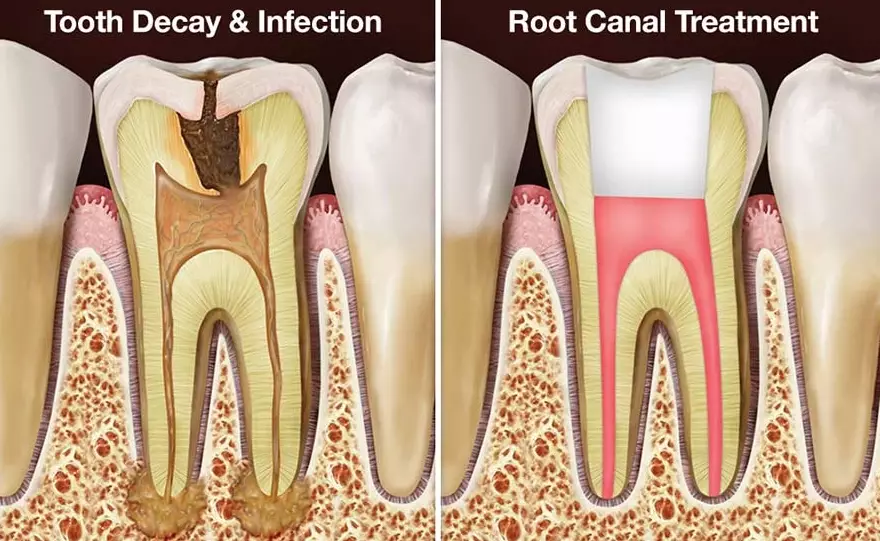
What’s Inside This Guide
Why Root Canal Teeth Can Change Color (It's Not Just Staining)
Most people think discoloration is just surface staining. With a root canal tooth, the problem usually starts from the inside. The tooth is no longer alive. Think of it like a piece of fruit—once the inside starts to break down, it can change the color of the skin.
The Internal Bleeding Theory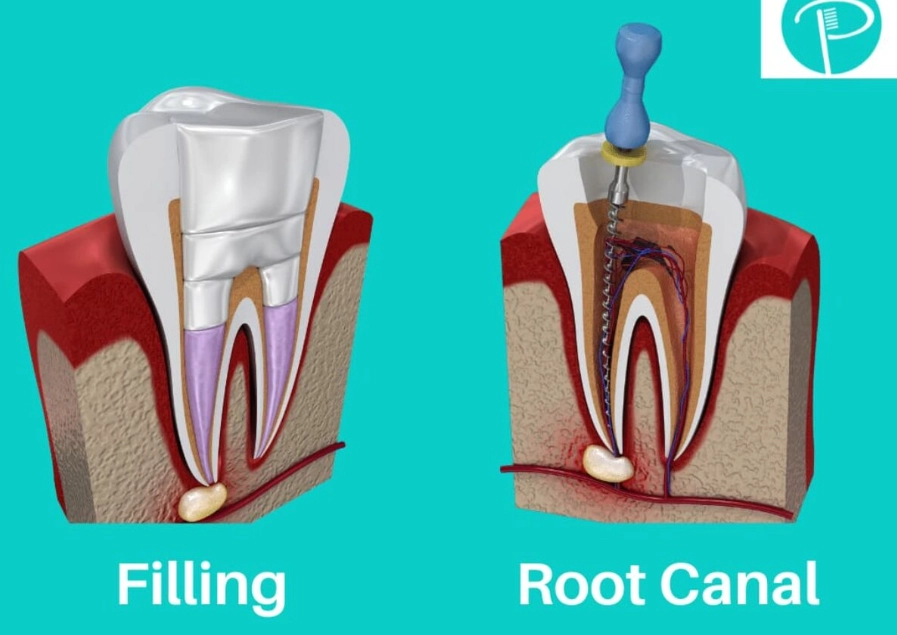
During the root canal, the dentist removes the inflamed or infected pulp—the living tissue inside your tooth containing nerves and blood vessels. Sometimes, tiny traces of blood and tissue debris remain inside the microscopic tubules of the dentin (the layer beneath the enamel). As this organic material breaks down over time, it can release pigments that stain the dentin from within. This is why the discoloration often appears greyish or dark yellow—it's literally an internal bruise.
The Filling Material Factor
To seal the cleaned root canals, dentists use a material called gutta-percha. Most modern versions are white, but some older or certain types of sealers can have a slight color that might show through over decades, especially if the enamel is thin. More critically, the cement used to bond a crown or filling can sometimes discolor if it's not perfectly matched or if it absorbs pigments.
How Can You Prevent Tooth Discoloration After a Root Canal?
Prevention is absolutely possible, and it starts in the dentist's chair. Not all dentists prioritize this, so it's something you might need to bring up.
Ask about the protocol. A meticulous dentist will take extra steps to minimize internal bleeding during the procedure and will thoroughly irrigate and clean the pulp chamber to remove all debris. Some even use special bleaching agents inside the tooth at the time of the root canal as a preventive measure, especially for front teeth.
The temporary filling matters. After the root canal, a temporary filling is placed. If this filling isn't perfectly sealed, saliva and bacteria can leak in, causing not just potential re-infection but also internal staining. A well-sealed, high-quality temporary is your first line of defense.
Don't delay the final restoration. This is critical. The root canal weakens the tooth structure. The standard of care is to protect it with a crown, usually within a few weeks to a couple of months. Leaving a root-canaled tooth with just a temporary or a simple filling for a long time invites fracture and increases the risk of internal contamination and discoloration. That crown acts as a protective, color-stable cap.
How to Fix a Discolored Tooth After Root Canal: Your 3 Main Options
So the tooth is already darker. Now what? Your choice depends on the severity of discoloration, the tooth's location, your budget, and the health of the remaining tooth structure. Let's break them down.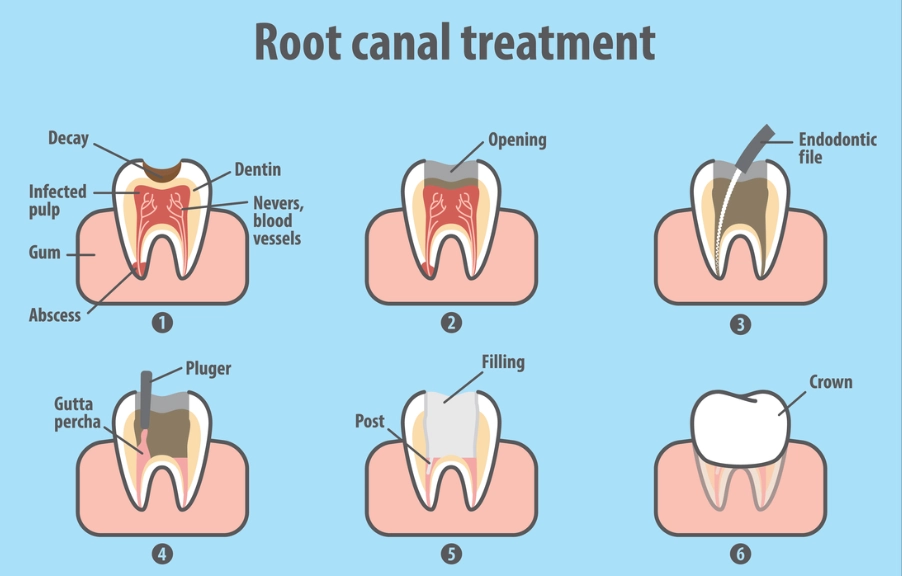
| Option | Best For | How It Works | Pros & Cons |
|---|---|---|---|
| 1. Dental Crown | Most common solution, especially for molars/premolars or severely discolored/weakened teeth. | The entire visible part of the tooth is filed down and capped with a custom-made porcelain or ceramic shell. | Pros: Extremely durable, restores strength, completely masks any color. Cons: More invasive (requires removing healthy tooth structure), higher cost, requires two visits. |
| 2. Dental Veneer | Front teeth with mild to moderate discoloration and otherwise good structure. | A thin layer of porcelain is bonded only to the front surface of the tooth, like a false fingernail. | Pros: Less tooth removal than a crown, highly aesthetic. Cons: Not as strong as a crown, may not mask very dark stains, requires healthy enamel for bonding. |
| 3. Internal (Walking) Bleach | Front teeth that are structurally sound but have internal, greyish discoloration. | The dentist re-opens the tooth from behind, places a bleaching gel inside the chamber, and seals it temporarily. Repeated over 1-3 visits. | Pros: Minimal invasion, preserves all natural tooth structure, can be very effective for specific stains. Cons: Not always predictable, may cause tooth brittleness or root resorption over very long periods (a debated risk). |
Here's a real-world scenario: Sarah had a root canal on her upper front tooth ten years ago. It gradually turned a dull grey. She was terrified she'd need a crown and lose her natural tooth shape. We evaluated and found the tooth was still strong. We performed internal bleaching over two appointments. The grey lifted significantly, matching her other teeth closely. We then placed a small, strong composite filling in the access hole. Total tooth structure preserved, natural look restored. A crown would have been overkill for her case.
Front Tooth vs. Back Tooth: A Big Difference in Appearance Concerns
Your concern level likely depends on which tooth had the work done.
Front Teeth (Incisors and Canines): This is the high-stakes zone. Any color mismatch is immediately visible. Dentists know this and will usually be more aggressive with preventive measures (like internal bleaching at the time of treatment) and will almost always recommend a final restoration that guarantees aesthetics—often a porcelain crown or veneer. The goal is an undetectable match.
Back Teeth (Premolars and Molars): While discoloration can still happen, it's less of a cosmetic emergency because these teeth aren't as visible. However, the structural concern is higher. A back tooth does a huge amount of chewing work. The primary reason for a crown here is function and prevention of fracture, not aesthetics. The crown will, as a happy side effect, also cover any discoloration completely. So the protocol is often more straightforward: root canal, then crown. The crown color is chosen to blend with your back teeth.
Your Root Canal Appearance Questions, Answered
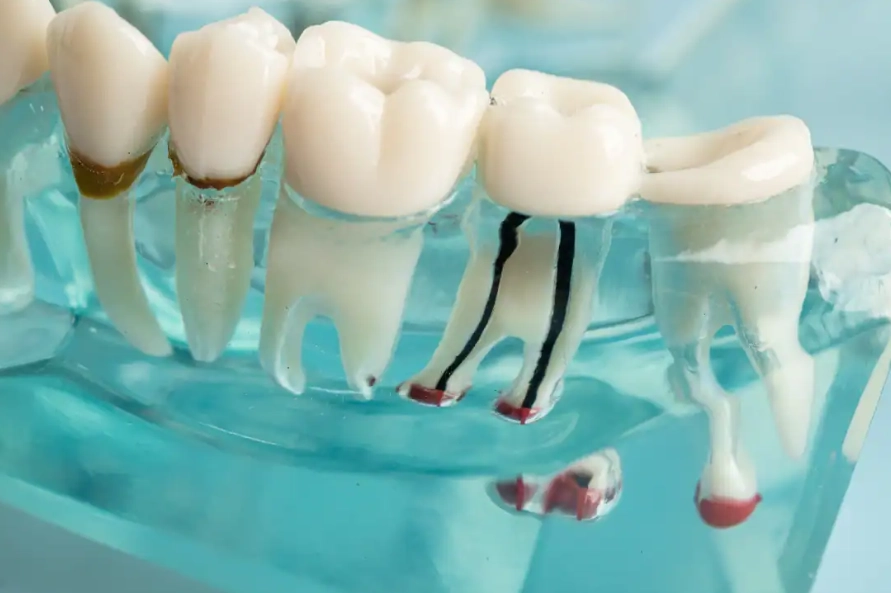 Is internal bleaching safe for my tooth in the long run?
Is internal bleaching safe for my tooth in the long run?The bottom line is this: A change in your tooth's appearance after a root canal is a common biological response, not a disaster. You have more control and more options than you might think. The path forward starts with a conversation with your dentist. Be specific about your concerns. Ask about the cause of the discoloration in your case. Discuss the pros and cons of each restoration option based on the long-term health of your tooth, not just the short-term color. With today's materials and techniques, there's no reason you can't have a healthy, pain-free tooth that also looks completely natural.
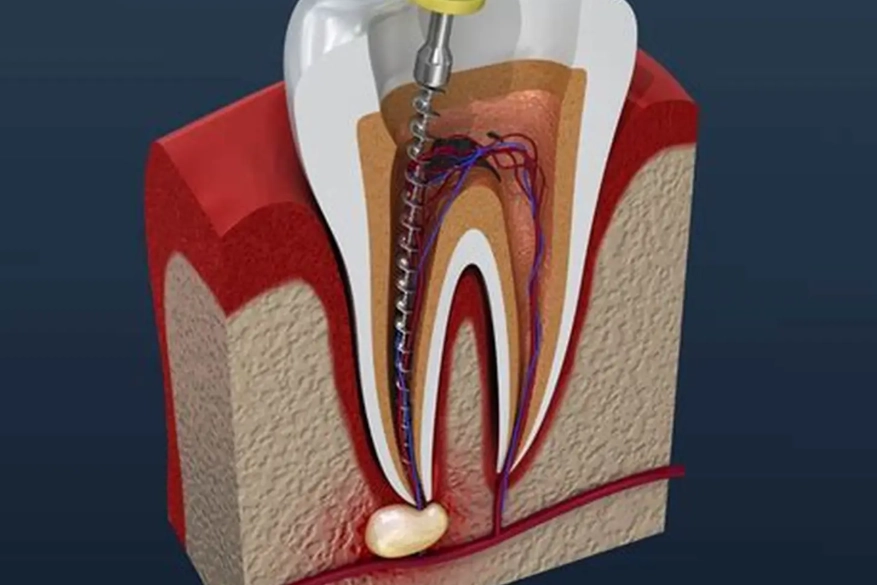 For more detailed information on the root canal procedure itself, you can refer to resources from the American Association of Endodontists, the leading professional organization for root canal specialists.
For more detailed information on the root canal procedure itself, you can refer to resources from the American Association of Endodontists, the leading professional organization for root canal specialists.