You know the drill: brush, floss, see the dentist. But what if I told you that one of the biggest threats to your oral health happens while you're unconscious? For over a decade in practice, I've seen patients meticulously care for their teeth yet struggle with persistent gum inflammation, unexplained cavities, or cracked molars. The missing piece often isn't in their bathroom cabinet—it's in their bedroom. The impact of poor sleep on oral health is a direct, biological chain reaction that most people, and even some dentists, overlook until significant damage is done.
What You'll Discover
The Mouth-Body Sleep Link You Can't Ignore
Think of your mouth not as a separate compartment, but as the front door to your body's overall health. When sleep suffers, the entire system goes on high alert, and your oral cavity is ground zero. The American Academy of Sleep Medicine and the American Dental Association have increasingly highlighted this overlap. Poor sleep—whether from insomnia, sleep apnea, or just chronic late nights—triggers stress hormones like cortisol, reduces saliva flow, and weakens immune function. Your mouth feels these changes first and hardest.
I had a patient, let's call him Mark, a 42-year-old software developer. He had great hygiene but kept getting cavities along his gumline. We checked his diet, his technique—everything. It wasn't until he mentioned his terrible sleep and constant dry mouth that it clicked. His mouth was a desert for 8 hours a night, perfect for bacteria to throw a cavity-causing party. We didn't just fix his teeth; we had to fix his sleep.
How Does Poor Sleep Lead to Dry Mouth?
This is the most immediate and damaging effect. Saliva is your mouth's natural defense system. It washes away food particles, neutralizes acids produced by bacteria, and contains minerals that repair early tooth decay.
During deep, restorative sleep, saliva production normally slows down a bit. But with poor-quality sleep, especially from mouth breathing (a common side effect of nasal congestion or sleep apnea), this reduction becomes extreme. You're not just sleeping with less saliva; you're actively drying out your tissues by breathing through your mouth all night.
The Domino Effect of Nighttime Dry Mouth: Less saliva → More acidic environment → Weakened tooth enamel → Faster plaque buildup → Increased risk for both cavities (especially at the gumline) and gum disease. It's a silent, nightly erosion.
Is It Just Snoring or Something More?
Mouth breathing and snoring are huge red flags. They're often signs of obstructed nasal airways or sleep-disordered breathing. If your partner says you snore, or you wake with a bone-dry mouth and a sore throat, don't just shrug it off. That dryness is a symptom of a problem that's also starving your brain of oxygen and straining your heart. Bringing this up with your dentist can be the first step to diagnosing sleep apnea—a condition dentists are often the first to suspect based on oral signs like a scalloped tongue (indentations from teeth) and a red, irritated throat.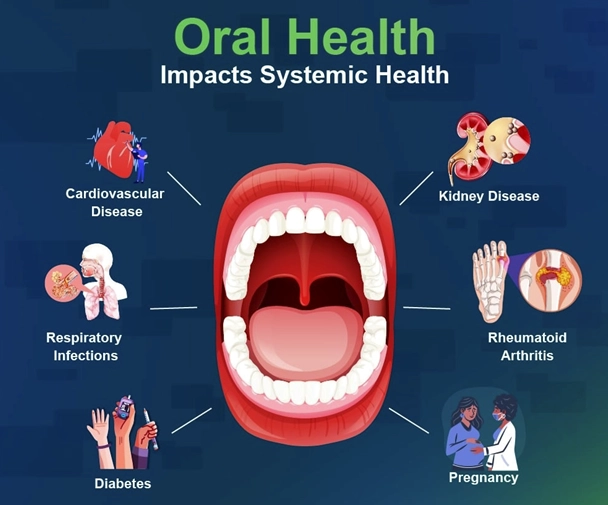
Teeth Grinding: Your Jaw's Midnight Panic Attack
Bruxism. Clenching and grinding. It's not just a bad habit; it's a physical manifestation of a nervous system that can't wind down. Poor sleep, particularly the lack of deep REM sleep, keeps your stress response activated. That tension has to go somewhere, and for many, it goes straight to the jaw muscles.
The force is unbelievable. People can exert up to 250 pounds of force on their teeth while grinding, compared to about 20-40 pounds during normal chewing. This isn't just about worn-down teeth. It leads to microfractures, sensitive teeth, headaches, and can even change the shape of your face by enlarging jaw muscles.
| Oral Health Problem | Direct Link to Poor Sleep | What You Might Notice |
|---|---|---|
| Increased Cavities | Reduced saliva flow (dry mouth) fails to neutralize acids. | Cavities at the gumline or between teeth, despite good brushing. |
| Gum Disease (Gingivitis/Periodontitis) | Weakened immune response allows harmful bacteria to flourish. | Gums that bleed easily, are puffy, or recede. |
| Bruxism & TMJ Pain | Heightened stress response and sleep arousal disorders. | Worn, flat teeth; jaw pain; morning headaches; sensitive teeth. |
| Canker Sores & Oral Ulcers | Immune dysregulation and increased local trauma from grinding. | More frequent, painful sores inside the mouth. |
| Bad Breath (Halitosis) | Dry mouth allows volatile sulfur compounds to build up overnight. | Persistent morning breath that doesn't resolve with brushing. |
A night guard from your dentist is a Band-Aid—it protects the teeth but doesn't stop the grinding. The real solution lies in improving sleep architecture and managing stress. Cognitive Behavioral Therapy for Insomnia (CBT-I) has shown more long-term promise for reducing bruxism than just a guard alone.
Sleep Deprivation and Your Gum's Defenses
Here's the subtle mistake most people make: they think gum disease is only about cleaning. It's also about healing. Your gums are living tissue constantly under mild attack by bacteria. Sleep is when your body repairs tissue and regulates inflammation.
Chronic short sleep—consistently getting less than 6-7 hours—throws your immune system into chaos. It overproduces inflammatory cytokines while underproducing the cells needed to fight specific infections. According to research highlighted by the National Sleep Foundation, this means the bacteria that cause gum disease (periodontitis) face a weakened defense team. The inflammation in your gums becomes chronic, leading to bone loss and tooth loss over time.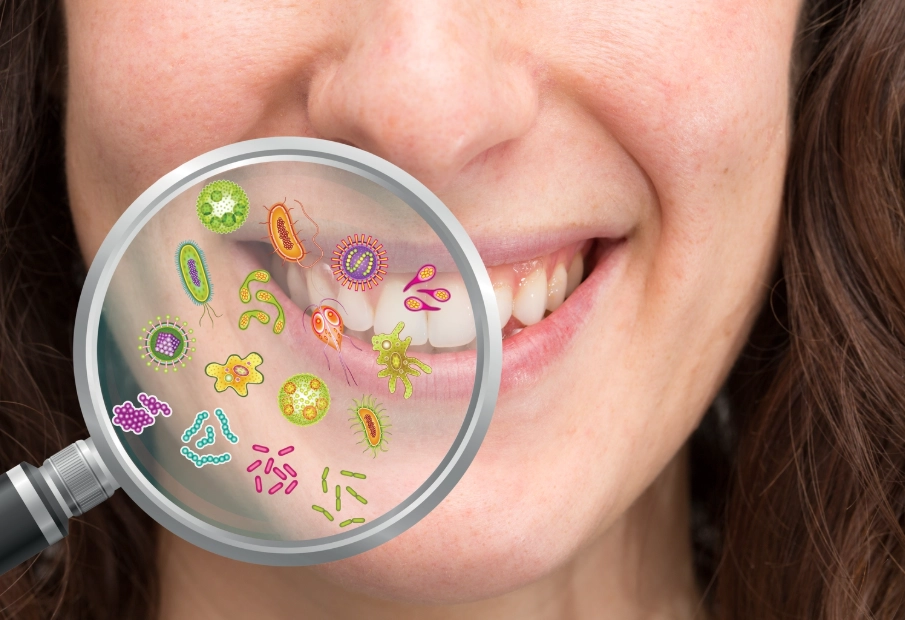
It creates a vicious cycle. Gum disease itself is an inflammatory condition that can further disrupt sleep through pain or systemic inflammation. You get stuck.
Your 3-Step Action Plan to Break the Cycle
This isn't about achieving perfect sleep overnight. It's about making targeted changes that address the oral-sleep connection directly.
Step 1: Audit Your Morning Mouth. For one week, the moment you wake up, ask yourself: Is my mouth desert-dry? Is my jaw sore? Do I have a headache? Does my breath smell worse than usual? This is your baseline data. Note it down.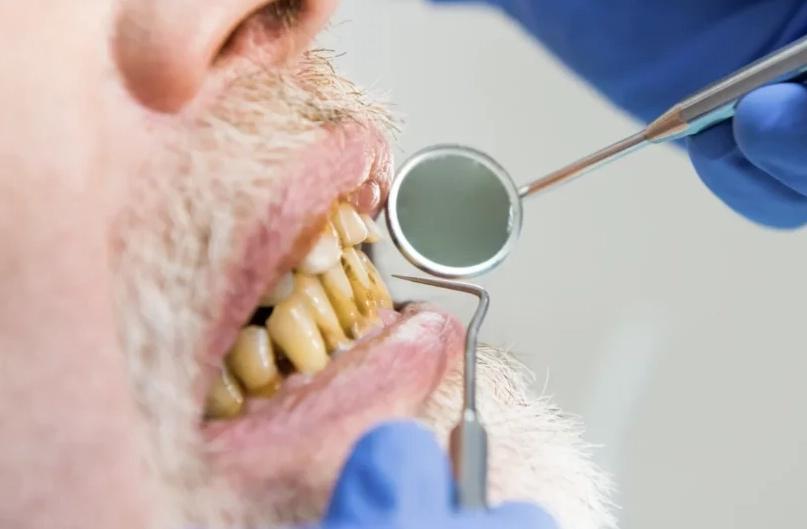
Step 2: Target the Dryness.
- Hydrate Strategically: Drink a large glass of water one hour before bed. Avoid sipping right before sleep to prevent disruptive bathroom trips.
- Humidify: Run a cool-mist humidifier in your bedroom. It adds moisture to the air you breathe all night.
- Consider a Dry Mouth Rinse: Use an alcohol-free, xylitol-containing mouthwash before bed. Xylitol helps inhibit bacteria, and the rinse provides a protective film. I often recommend brands like Biotene.
Step 3: Talk to Both Your Dentist AND Your Doctor. Bring your "morning mouth" notes to your dentist. Describe your sleep. Ask specifically: "Do you see signs of dry mouth or grinding? Could sleep apnea be a factor?" Based on oral signs (like a large tongue, scalloping, or a small airway), they may recommend a sleep study. Treating sleep apnea with a CPAP machine, for instance, can eliminate nighttime dry mouth and dramatically reduce grinding almost instantly.
Your Top Questions Answered
I use a night guard for grinding, but I'm still tired. Is it really helping?
Can improving my sleep actually reverse gum disease?
I breathe through my mouth at night because my nose is always stuffy. What can I do besides a CPAP?
Are there specific signs my dentist should look for that link my oral issues to sleep?