That dull, persistent ache deep in the back of your jaw. The feeling that your gums are swollen and angry. Maybe it hurts to chew, or you even taste something foul. If you're in your late teens to twenties, there's a good chance you're getting a firsthand introduction to a wisdom tooth infection, or what dentists call pericoronitis. It's not just a minor inconvenience—it's a sign that something is seriously wrong in a hard-to-reach part of your mouth. I've seen too many patients wait it out, hoping it'll vanish, only to end up in the emergency dental chair with a face swollen like a chipmunk's. Let's cut through the confusion and talk about what's really happening, what you should do right now, and what your long-term options are.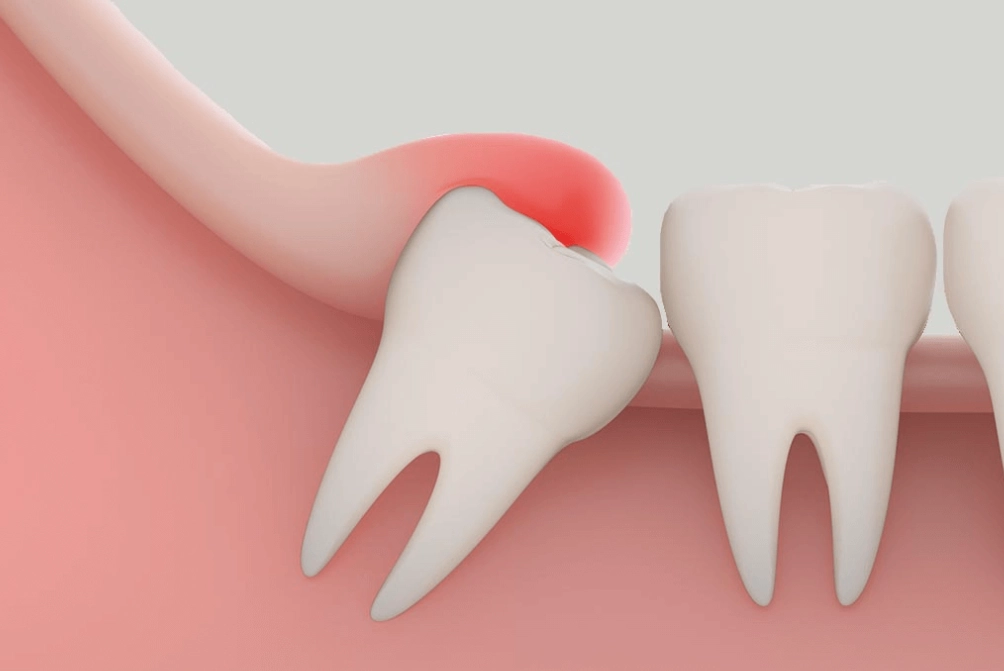
What You'll Find in This Guide
- What Exactly Is a Wisdom Tooth Infection?
- Signs You Have an Infection (Not Just Normal Pain)
- What to Do RIGHT NOW for Relief (The Safe Way)
- How to Treat a Wisdom Tooth Infection: Your Options Explained
- What Recovery Really Looks Like After Treatment
- Can You Prevent It? Realistic Strategies That Work
- Your Top Wisdom Tooth Infection Questions, Answered
What Exactly Is a Wisdom Tooth Infection?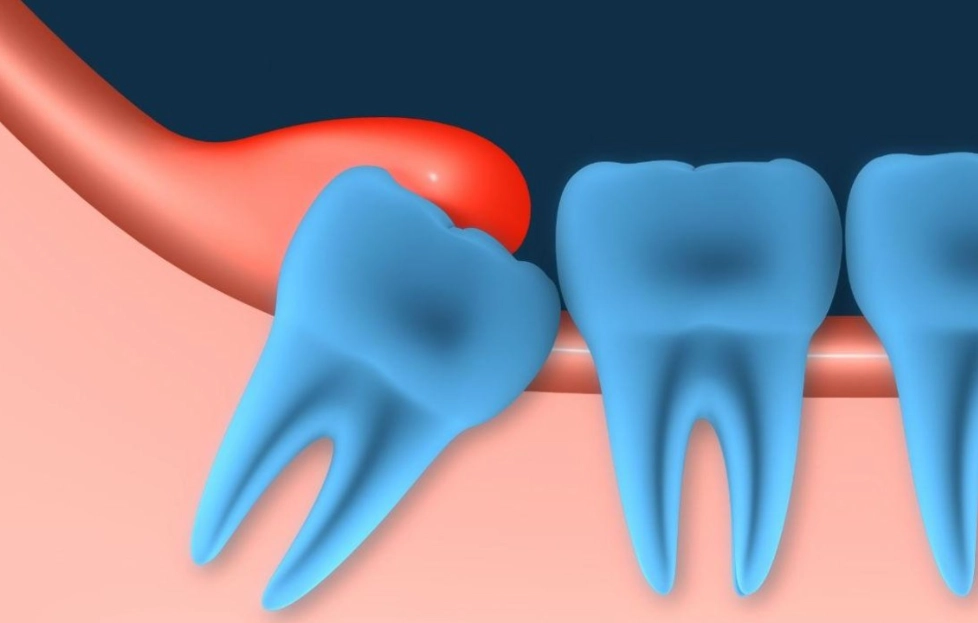
Pericoronitis. It's the technical term, and it describes inflammation and infection of the gum tissue surrounding a partially erupted tooth—almost always a wisdom tooth. Here's the simple mechanics: your wisdom tooth tries to come in, but there's no room. It gets stuck (impacted). It might only poke through the gums a little. This creates a perfect trap: a flap of gum tissue, called an operculum, hangs over the tooth. Food, bacteria, and plaque get packed under that flap. You can't brush or floss it effectively. It becomes a warm, dark, food-filled petri dish, and infection is the inevitable result.
The American Dental Association notes that impacted third molars (wisdom teeth) are a common source of oral infection. It's not a question of if it will become a problem for many people, but when.
Signs You Have an Infection (Not Just Normal Pain)
How do you know it's an infection and not just the tooth pushing through? Normal eruption discomfort is mild and intermittent. An infection announces itself loudly and gets worse.
Pain that radiates. It starts at the tooth but can spread to your ear, your throat, the entire side of your head. It's often a deep, throbbing ache that painkillers barely touch.
Swollen, angry gums. The tissue around the tooth turns red, shiny, and extremely tender to the touch. The swelling can be visible on the outside of your face along the jawline.
Bad taste or breath. This is a dead giveaway. The infection produces pus, which has a distinct, foul odor and taste that lingers no matter how much you brush.
Difficulty opening your mouth (trismus). The inflammation affects the jaw muscles, making it hard and painful to open wide. Trying to eat a sandwich becomes a challenge.
Swollen lymph nodes. Check under your jaw and in your neck. If they're tender and feel like small, firm beans, your immune system is fighting hard.
Fever and general malaise. If the infection is significant, your whole body gets involved. You might feel run-down, feverish, and just plain sick.
What to Do RIGHT NOW for Relief (The Safe Way)
You feel the pain coming on. It's 10 PM. Your dentist's office is closed. Here's your action plan, ranked by effectiveness and safety.
Salt Water Rinses are your best friend. Not a quick swish. Dissolve half a teaspoon of salt in a warm glass of water. Gently but thoroughly swish it around the affected area for 30 seconds, 3-4 times a day. The warmth increases blood flow, and the salt draws out some of the fluid causing swelling. It's simple, but it works.
Over-the-counter pain relief. Ibuprofen (Advil) is typically better than acetaminophen (Tylenol) here because it reduces both pain and inflammation. Follow the package directions.
Be meticulous with oral hygiene—gently. Try to brush very carefully around the area. Use a soft-bristled brush. An antibacterial mouthwash (like one containing chlorhexidine, if you have it) can help reduce bacterial load. Avoid alcohol-based mouthwashes as they can irritate.
What NOT to do. Do not place aspirin directly on the gums—it can cause a chemical burn. Do not aggressively poke or try to "clean under the flap" with sharp objects—you'll just drive bacteria deeper and cause more trauma. Do not rely on "numbing" gels for more than a day or two; they mask the problem while it gets worse.
These are temporary measures. They manage symptoms but do not cure the underlying infection. For that, you need professional help.
How to Treat a Wisdom Tooth Infection: Your Options Explained
Once you see a dentist or oral surgeon, the treatment path depends on the severity and your long-term dental health. The goal is first to control the acute infection, then to address the cause so it doesn't return.
Step 1: Controlling the Active Infection
If there's significant swelling and pus, you'll likely need a course of antibiotics. Common ones include amoxicillin or clindamycin. Critical point: Antibiotics alone are not a cure. They calm the infection down, making it safer and more comfortable to perform the necessary dental procedure. The infection WILL come back if the source (the trapped debris under the gum flap) isn't removed.
The dentist may also perform an irrigation and debridement. Using a specialized syringe, they flush out the debris and bacteria from under the gum flap. This can provide instant, dramatic relief. Sometimes, they may make a small incision to drain an abscess.
Step 2: The Definitive, Long-Term Solutions
After the acute phase is managed, you have decisions to make. Here’s a breakdown of your main options:
| Option | What It Is | Best For | Major Consideration |
|---|---|---|---|
| Wisdom Tooth Removal (Extraction) | Surgical removal of the problematic wisdom tooth. | Teeth that are fully or partially impacted, recurrent infections, or causing crowding/damage to other teeth. | Permanent solution. Prevents all future problems with that tooth. Requires a recovery period. |
| Operculectomy | Minor surgery to remove the gum flap (operculum) covering the tooth. | A fully erupted, healthy wisdom tooth that is just plagued by the gum flap trapping food. | Less invasive than extraction. The flap can sometimes grow back, and it doesn't address underlying impaction. |
| Non-Surgical Management & Monitoring | Aggressive hygiene, regular professional cleanings, and using a water flosser (like a Waterpik) to clean under the flap. | Very minor, infrequent episodes in a patient who is not a good surgical candidate, or for a tooth that is almost fully in and correctly positioned. | Requires extreme diligence. The risk of recurrent infection remains. Often a temporary measure. |
Most oral surgeons and general dentists will lean towards extraction for a tooth that has already caused one significant infection. The data from the National Institutes of Health shows a high rate of recurrence with other methods. The logic is simple: you remove the architectural flaw that causes the problem.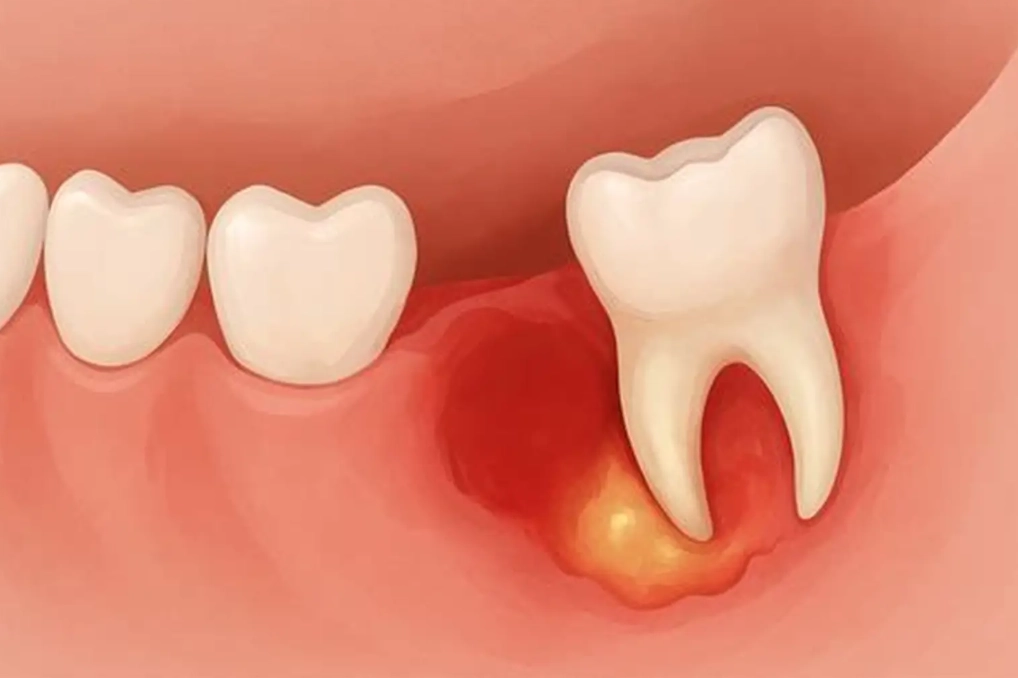
What Recovery Really Looks Like After Treatment
If you have an extraction, knowing what to expect eases a lot of anxiety. The first 24-48 hours are about managing swelling and bleeding.
Bleeding: You'll bite on gauze. Change it as directed. Some oozing is normal. It's not like a cut on your hand; the saliva mixes with a little blood and looks worse than it is.
Swelling: This peaks around day 2-3. Use an ice pack on the outside of your cheek (20 minutes on, 20 minutes off) for the first day. After 48 hours, switch to gentle warm compresses to encourage healing.
Diet: Stick to cool, soft foods. Yogurt, pudding, smoothies (no straws!), mashed potatoes, scrambled eggs. The suction from a straw can dislodge the blood clot that's forming in the socket, leading to a painful complication called dry socket.
Pain: You'll have prescription pain medication or instructions for OTC meds. Take them before the local anesthetic fully wears off to stay ahead of the pain.
The biggest mistake I see? People think they feel great on day 3 and go eat chips or vigorously rinse. Then they're in my office on day 4 with throbbing dry socket pain. Take it easy for a full week. Follow your surgeon's post-op instructions to the letter.
Can You Prevent It? Realistic Strategies That Work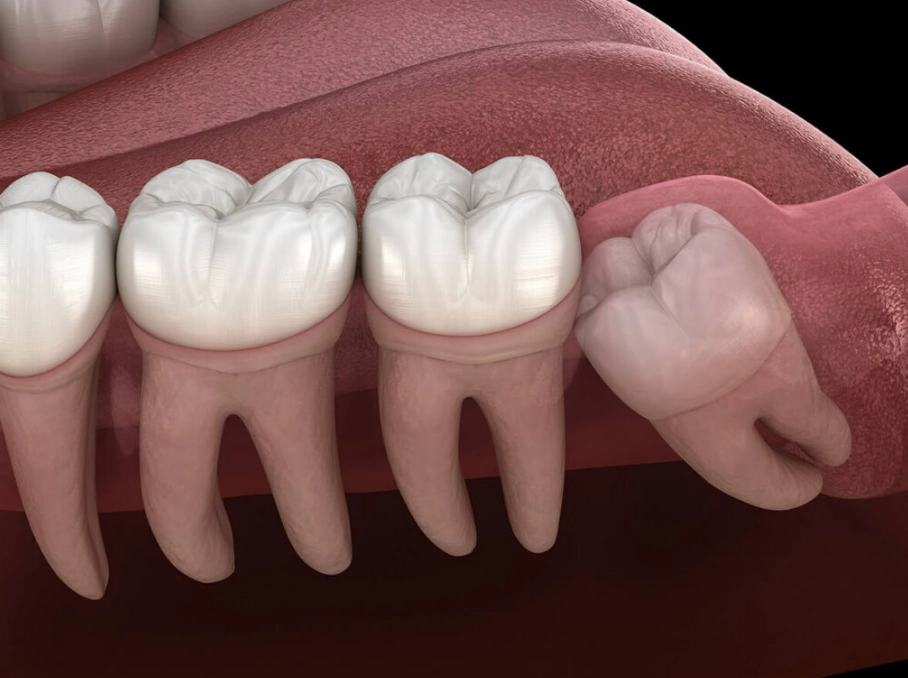
If your wisdom teeth are still lurking under the gums and haven't caused trouble yet, can you prevent an infection? Sometimes, but not always.
Get a panoramic X-ray. This is non-negotiable. By your late teens, a dentist can see the position, angle, and development of your wisdom teeth. They can predict with reasonable accuracy if they will likely cause problems. Proactive removal of clearly impacted teeth before they infect is often the smartest prevention.
If you're keeping them, hygiene is everything. When they start to erupt, add a water flosser to your routine. The targeted stream can clean under gum flaps better than anything else. Use an angled toothbrush (like a monojet brush) to reach the very back surfaces.
Pay attention to early signs. A little tenderness or a feeling of tightness in the back of your jaw might be the first signal. Don't ignore it. Ramp up the salt water rinses and be extra vigilant with cleaning.
Let's be honest, though. For many people, especially with fully impacted teeth, infection is almost a biological certainty. Prevention, in those cases, means preventing the emergency by dealing with the tooth electively on your own schedule.
Your Top Wisdom Tooth Infection Questions, Answered
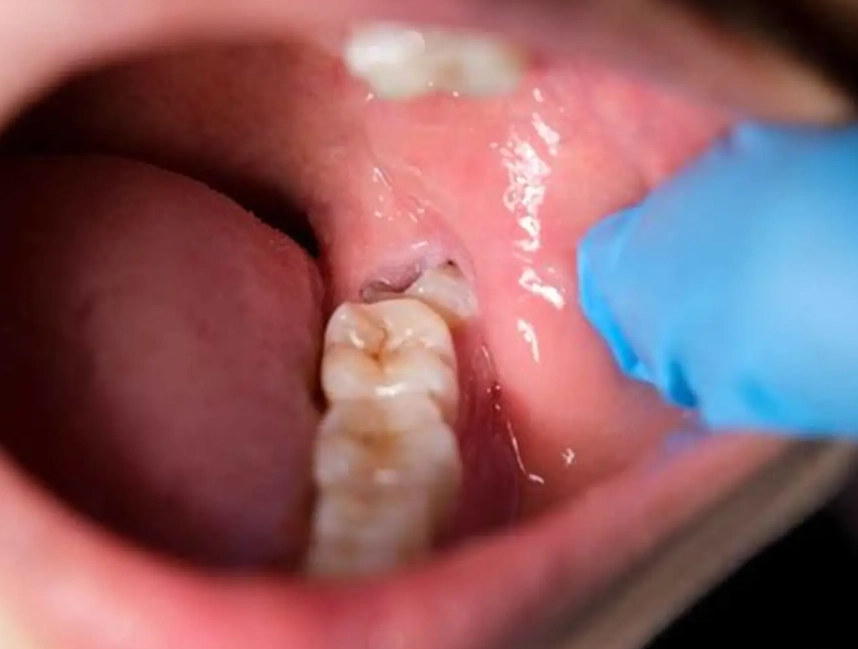 How can I tell if my pain after wisdom tooth extraction is normal or a sign of a new infection?
How can I tell if my pain after wisdom tooth extraction is normal or a sign of a new infection?