That nagging pain in your back tooth won't go away. Your dentist says you have a deep cavity or an infection reaching the nerve, and now they're talking about a root canal on a molar. Your mind immediately goes to two things: pain and cost. You've heard the horror stories. You're sitting there wondering, point blank, is a root canal worth it?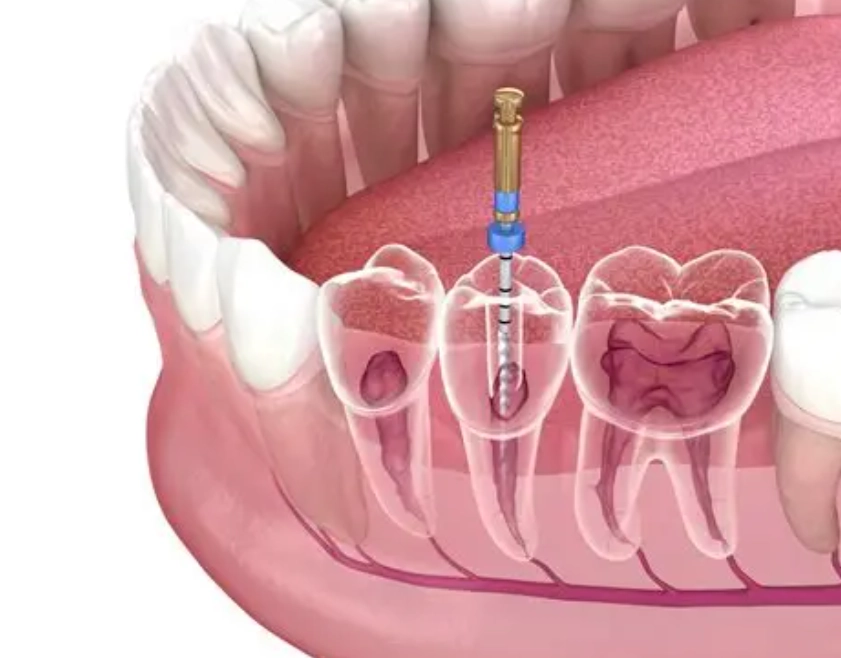
Let's cut through the noise. As someone who's seen hundreds of these cases, the short answer is: usually, yes. But that "usually" carries a lot of weight. The real question isn't just about surviving the procedure. It's about whether saving that specific molar with a root canal treatment is a smart, long-term investment in your health and your wallet compared to the alternative—pulling it out.
This guide won't just list facts. We'll compare, calculate, and look at scenarios most articles skip. We'll talk about when it might *not* be the best move. Let's figure this out together.
What's Inside This Guide
Root Canal vs. Tooth Extraction: The Real Breakdown
This is the core of your decision. It's not root canal vs. nothing. It's root canal (saving the tooth) vs. extraction (removing it). Let's put them side-by-side.
| Factor | Root Canal Therapy (Saving the Molar) | Tooth Extraction (Removing the Molar) |
|---|---|---|
| Primary Goal | Preserve your natural tooth structure and function. | Remove the source of infection/pain entirely. |
| Initial Cost | Higher upfront (procedure + crown). | Significantly lower upfront cost. |
| Long-Term Cost | One-time major investment. With proper care, the tooth can last a lifetime. | Seems cheap now, but often leads to higher future costs (implants, bridges, orthodontics). |
| Procedure & Recovery | Multi-visit, non-surgical. Mild soreness for a few days. | Single, often quicker visit. Healing of extraction site takes 1-2 weeks. |
| Impact on Oral Health | Maintains bone, prevents neighboring teeth from shifting, preserves full chewing function. | Bone loss in the jaw over time. Neighboring teeth can tilt, opposing tooth can over-erupt. Chewing efficiency drops. |
| Success Rate | Very high, around 95% when followed by a proper crown according to the American Association of Endodontists. | 100% at removing the tooth. 100% at creating a new problem (the gap). |
Here's the perspective most miss: extraction is not a final solution; it's the start of a new problem. That empty space is like removing a foundational brick from a wall. Things shift.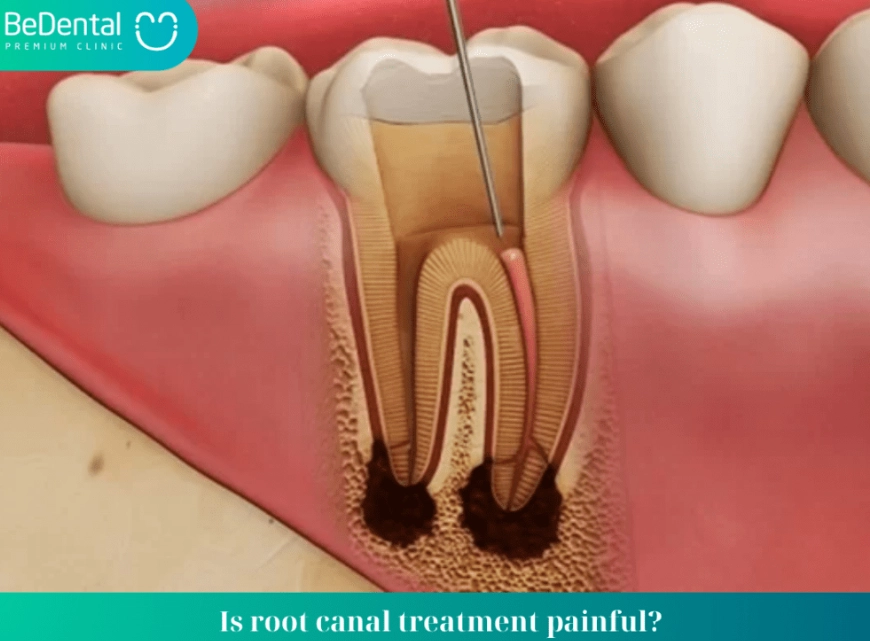
I had a patient, let's call him Mark. He had a lower molar extracted ten years ago because the root canal quote scared him. Fast forward to now, the tooth above it had dropped down, the teeth next to the gap had tilted, and he was getting food stuck constantly, leading to new cavities. He came to me asking about an implant, which cost three times what the original root canal and crown would have.
That's the hidden math.
When Extraction Might Be the Smarter Choice
I'm not a "save every tooth at all costs" dentist. There are clear cases where an extraction is the more pragmatic, worth-it choice:
- The Tooth is Too Far Gone: Severe vertical fracture deep under the gum, or massive decay that leaves no solid structure for a crown to anchor onto.
- Severe Gum/Bone Disease: If the bone supporting the tooth is mostly destroyed from advanced periodontal disease, saving the tooth is a doomed, expensive battle.
- Strategic Non-Critical Molar: Sometimes, if a patient is already missing the opposing molar (the one it chews against), saving a heavily compromised tooth with a complex root canal may offer little functional benefit. This is a nuanced call.
- Overwhelming Financial or Medical Constraint: When the cost is truly prohibitive and no financing is possible, or a patient's health makes a multi-visit procedure risky.
How Much Does a Molar Root Canal Cost? Unpacking the Numbers
Let's talk money, because this is a huge part of the "worth it" equation. People get sticker shock from a single number without understanding what it includes.
A molar root canal cost isn't one fee. It's typically three parts:
- The Root Canal Treatment Itself: The endodontist or general dentist cleans and seals the canals. Molars are complex (3-4 roots), so this is the most expensive type.
- The Core Buildup: After the root canal, the tooth's center is hollow. A post and filling material are often placed to give the crown something to grip.
- The Dental Crown: This is NON-NEGOTIABLE for a molar. A root-canaled tooth is brittle. A crown is the helmet that protects it from the immense chewing forces. Skipping the crown is the #1 reason for root canal failure I see.
Realistic Total Cost Range (U.S.): For a molar treated by a general dentist, you're looking at $1,200 - $1,800 for the root canal, plus $1,000 - $1,500 for the crown. Totals often land between $2,200 and $3,300. An endodontist (specialist) may charge 20-50% more for the root canal portion. Geographical location dramatically affects this.
Now, compare that to the alternative path: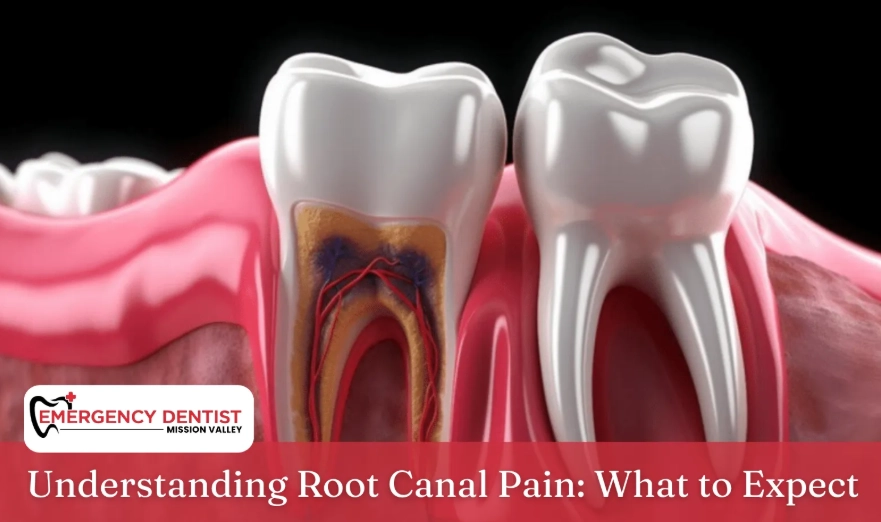
- Extraction Only: $150 - $400. Seems like a no-brainer, right? But wait.
- Extraction + Dental Implant (the standard of care to replace a molar): $3,000 - $6,000+.
Extraction + Bridge: $2,500 - $5,000.
Extraction + Do Nothing: $0 upfront, but potential future costs for orthodontics, cavities in shifted teeth, and TMJ issues from altered bite.
Suddenly, the $2,500-$3,500 root canal/crown package looks like a long-term bargain to preserve your original biological part.
Navigating Dental Insurance
Most plans cover root canals at 50-80% and crowns at 50%. They often have annual maximums ($1,000-$1,500 is common). This means you might hit your max with this procedure. Get a pre-treatment estimate. Understand that insurance companies base payments on "UCR" fees, which are often lower than actual fees. Be prepared to pay the difference.
What Actually Happens During a Molar Root Canal?
The fear of the unknown is huge. Knowing the steps demystifies it.
Visit 1: Diagnosis and Prep. Numbness is paramount. We use stronger numbing for infected teeth because the acidity can interfere. Once you're profoundly numb (you shouldn't feel sharp pain), a rubber dam is placed. This is a small sheet that isolates the tooth. It's not just for moisture control; it's a major safety and success factor that many patients don't know about.
The Work: A small opening is made in the tooth's top. Using tiny files, the infected or dead pulp (nerve tissue) is removed from each root canal. The canals are disinfected, shaped, and then filled with a rubber-like material called gutta-percha. The access hole is sealed with a temporary filling.
You might feel pressure, but not pain. The modern procedure, with good anesthesia, is far more boring than the old tales suggest. The real pain was the infection you walked in with.
Visit 2: The Crown. This happens a few weeks later, usually with your general dentist. The temporary filling is removed, a buildup is done, the tooth is prepared, impressions are taken, and a temporary crown is placed. At Visit 3, the permanent crown is cemented.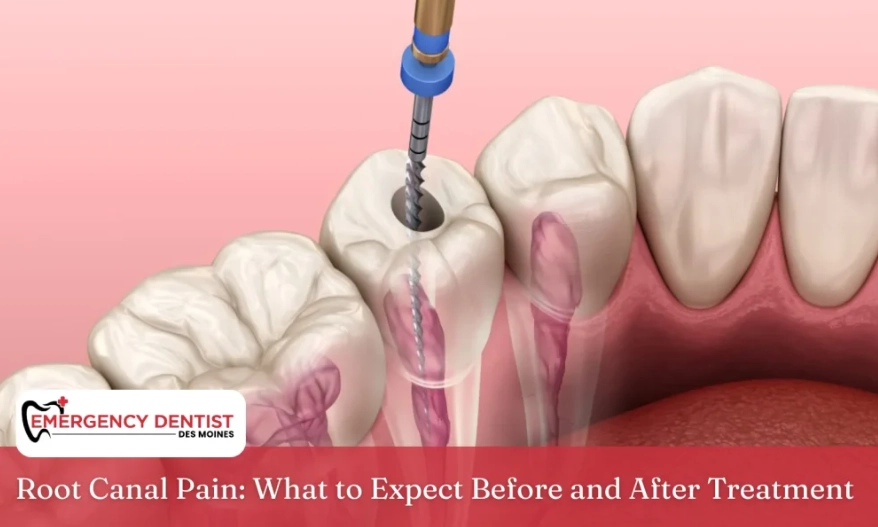
How to Decide If a Root Canal Is Worth It For You
Ask yourself and your dentist these questions:
- What's the long-term prognosis? Ask for the success rate estimate for YOUR specific tooth based on X-rays. Is there a crack? How much solid tooth remains?
- Can I commit to the crown? If you can't afford or commit to the protective crown, the root canal itself is often a waste of money. The tooth will likely fracture.
- What's the alternative plan—really? Don't let "we'll just take it out" be the end of the conversation. Ask: "And then what? What are the consequences and costs of leaving that space empty in 5 years? What are the replacement options and their costs?"
- Who is doing the procedure? For complex molars (curved roots, previous canals), a referral to an endodontist might be worth the extra cost for higher expertise and specialized equipment like a dental microscope.
Your Root Canal Questions, Answered
 How long will a root-canaled molar last? Is it a permanent fix?
How long will a root-canaled molar last? Is it a permanent fix?So, is it worth doing a root canal on a molar? For the vast majority of people facing a salvageable tooth, the answer leans heavily toward yes. It's an investment in preserving your natural anatomy, preventing a cascade of future dental problems, and often proves to be the most cost-effective long-term path. The value isn't just in the procedure itself, but in everything it allows you to keep.
Get the diagnosis. See the X-ray. Ask the hard questions about prognosis and alternatives. Then, you can move past the fear and make a decision based on facts, not folklore.