Let's cut straight to the point. The idea of a root canal being a torturous experience is a decades-old myth. Honestly, I get it. The phrase itself sounds invasive and scary. But here's the truth you need to hear: modern root canal treatment should not be painful during the procedure. The severe pain people associate with it is usually the toothache that leads you to the dentist in the first place. The treatment itself is the solution to that pain. I've seen countless patients walk out surprised, saying, "That was it?" The real story is about how dental technology and anesthesia have evolved to make this a routine, comfortable procedure.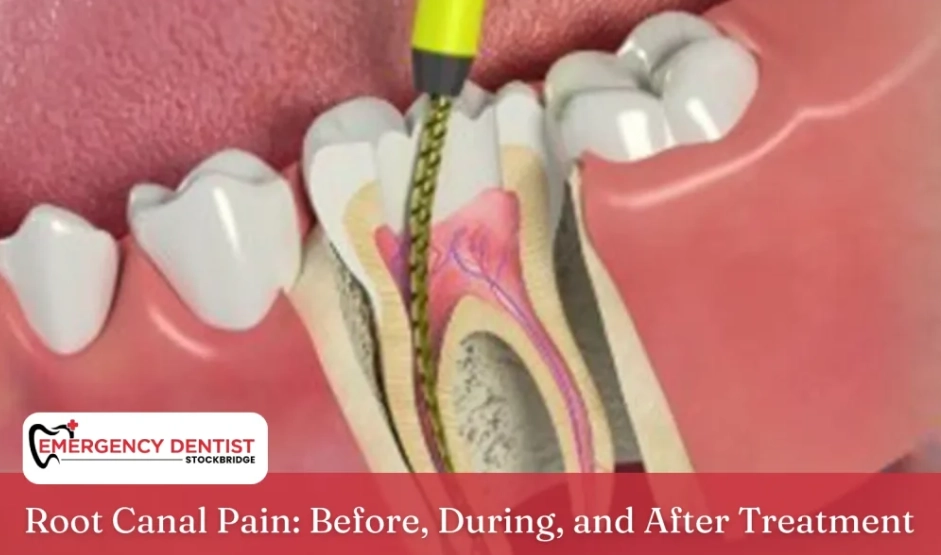
What's Covered in This Guide
Myth vs. Reality: Where Does the Pain Really Come From?
Think of an infected tooth like a tiny, pressurized balloon inside your jawbone. The pulp—the living tissue with nerves and blood vessels—gets inflamed or infected due to deep decay, a crack, or repeated dental work. That inflammation has nowhere to go, so it presses against the rigid walls of your tooth and bone. That pressure is what causes that intense, throbbing, "I need to do something about this" kind of pain.
The root canal procedure relieves that pressure by removing the inflamed pulp, cleaning the space, and sealing it. So, you're not walking into pain; you're walking out of it.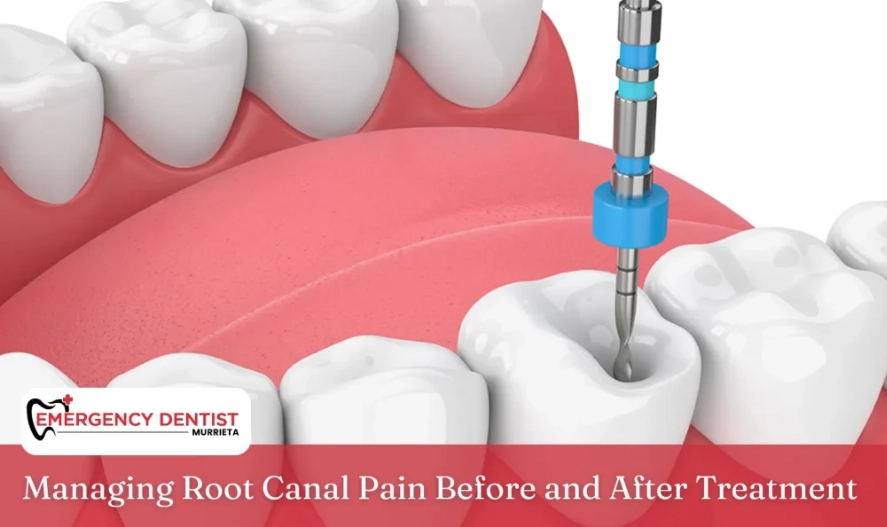
Where the myth persists is in the memory of older techniques and, frankly, some less-than-optimal patient experiences. Local anesthesia has improved dramatically. We now have better drugs, better delivery systems (like computer-controlled devices), and a deeper understanding of anatomy to ensure you're completely numb.
The fear isn't entirely unfounded—it's just outdated. Here’s how things have changed.
| Aspect | The Old Fear ("Then") | Modern Reality ("Now") |
|---|---|---|
| Anesthesia | Basic numbing agents; sometimes ineffective on severely infected teeth. | Advanced anesthetics (like Articaine) that work even in infected areas. Techniques like intraosseous injections can numb a tooth when standard methods struggle. |
| Pain During Procedure | Potential for feeling pressure or occasional sharp sensations. | The goal is zero pain. You should only feel vibration, pressure, or movement. Any sharp sensation means you tell your dentist, and they add more anesthetic. |
| Technology | Manual files, less precise X-rays. | Electronic apex locators to precisely measure root length, rotary instruments that work faster and smoother, digital 3D imaging for complex cases. |
| Post-Op Pain | Often significant soreness, managed with limited options. | Mild to moderate soreness for a few days, easily managed with over-the-counter ibuprofen or acetaminophen for most people. |
How Does a Root Canal Actually Work? A Step-by-Step Walkthrough
Knowing what will happen is the best way to disarm anxiety. Let me walk you through a typical appointment for a molar root canal, which is the most complex scenario.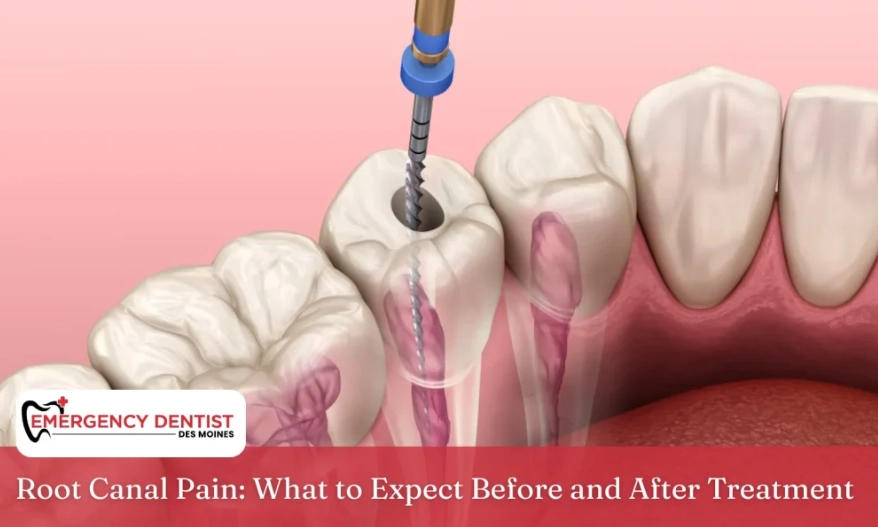
Step 1: The Numbing Process
This is the most critical part for your comfort. Your dentist will first apply a topical gel to numb the gum surface. The actual injection feels like a tiny pinch or pressure for a few seconds. For a severely inflamed tooth, they might do a "ligamentary injection" first to calm the main nerve before the deeper block. The key is patience—we wait a full 5-10 minutes to let the anesthetic diffuse completely. A good sign it's working is your lip or tongue feeling fat and tingly.
Step 2: Isolation and Access
A small rubber sheet called a dental dam is placed over the tooth. This isn't just for moisture control; it's a major safety and comfort feature. It keeps everything clean and prevents any tiny instruments from going down your throat. You can still breathe and swallow normally. Then, a tiny opening is made in the top of the tooth. If the pulp is alive, you feel nothing. If it's necrotic (dead), you already couldn't feel it anyway.
Step 3: Cleaning and Shaping
This is the core of the procedure. Using very small, flexible files, the dentist removes the infected pulp tissue and shapes the root canals. You'll hear a faint buzzing or humming sound and feel vibrations. It's similar to the feeling of a deep filling, just longer. The use of a electronic apex locator is a game-changer—it beeps when the file reaches the exact end of the root, eliminating guesswork and reducing post-op discomfort.
Step 4: Disinfection and Filling
The canals are flushed with antibacterial solutions. Then, they are dried and filled with a biocompatible rubber-like material called gutta-percha. This seals the space to prevent re-infection.
Step 5: The Temporary Filling
The access hole is sealed with a temporary filling. You'll need to return later for a permanent crown, as a root-canaled tooth is more brittle and needs protection.
The entire process for a single-rooted tooth can take 30-60 minutes. A molar might take 90 minutes or more. You're just lying there, probably listening to music or a podcast through your headphones.
Your Pain Management Toolkit: Before, During, and After
Managing discomfort is a multi-stage strategy. It's not just about the needle.
- Before the Appointment: If you're in severe pain, your dentist might prescribe an antibiotic or a short course of anti-inflammatory medication to reduce the infection and inflammation before treatment, making anesthesia more effective. Get a good night's sleep. Avoid caffeine that day, as it can heighten anxiety.
- Communication is Your Superpower During: You are in control. Agree on a hand signal (like raising your left hand) to signal you need a break or feel any sharpness. Don't suffer in silence thinking you have to tough it out. A good dentist wants to know.
- The Immediate Aftermath (First 24-48 hours): Your tooth and surrounding jawbone will feel tender, like you've been pressing on a bruise. This is normal inflammation from the procedure itself, not the infection. This is where pain is most common, and it's completely manageable.
- Medication Protocol: Take ibuprofen (Advil) before the anesthetic fully wears off. I recommend 400-600mg if you can take NSAIDs. This blocks the inflammatory prostaglandins before they cause significant pain. Pair it with acetaminophen (Tylenol) for a synergistic effect, as recommended by studies from sources like the American Dental Association. Follow your dentist's specific instructions.
- The Ice Pack Trick: Apply an ice pack to the outside of your cheek in intervals (15 minutes on, 15 minutes off) for the first few hours. It makes a huge difference.
- Soft Diet: Stick to soups, yogurt, mashed potatoes. Avoid chewing on that side completely.
The Realistic Recovery Timeline: What to Expect Day by Day
Let's set realistic expectations so you're not worried by normal healing.
Day of Treatment: Numbness wears off in 2-4 hours. Soreness sets in. Take your first dose of pain relievers during this window. Rest.
Day 2-3: Peak of soreness, but it should be noticeably improving each day. You can usually resume light chewing on the other side. The sensation is more of a dull ache.
Day 4-7: Most tenderness is gone. You might only feel it when you bite down hard directly on the tooth. This is because the ligament around the tooth root is still healing.
Beyond 1 Week: Any lingering sensitivity to biting should resolve. If you have a persistent, throbbing pain or swelling that increases after a few days, call your dentist. This isn't normal healing and could indicate a need for further evaluation.
Your Top Root Canal Pain Questions, Answered
 Is the pain after a root canal worse than the original toothache?
Is the pain after a root canal worse than the original toothache?So, is root canal treatment painful? The procedure itself, when done with modern care, is designed to be pain-free. The recovery involves manageable soreness, not agony. The greatest pain is often the fear and the toothache that brought you in. By understanding what truly happens and communicating with your dental team, you can replace that fear with relief, knowing you're finally fixing the problem.