Let's be honest. That reminder card for your dental cleaning can feel like a summons for mild torture. You sit in the chair, hear the whirring tools, and brace for those sharp zings of pain. It’s a common dread. But here’s the thing: while some sensitivity is normal, significant pain during a routine cleaning is your mouth sending you a clear signal. It’s not just "bad luck" or a "low pain tolerance." It’s specific, often preventable, and understanding it is the first step to a more comfortable visit.
I've been on both sides of this—as a patient who used to white-knuckle the armrests and later, through extensive research and conversations with dental professionals, as an observer of the nuances many blogs miss. The standard answer—"you have gum disease"—is often correct but incomplete. The real story is more about inflammation, technique, and communication.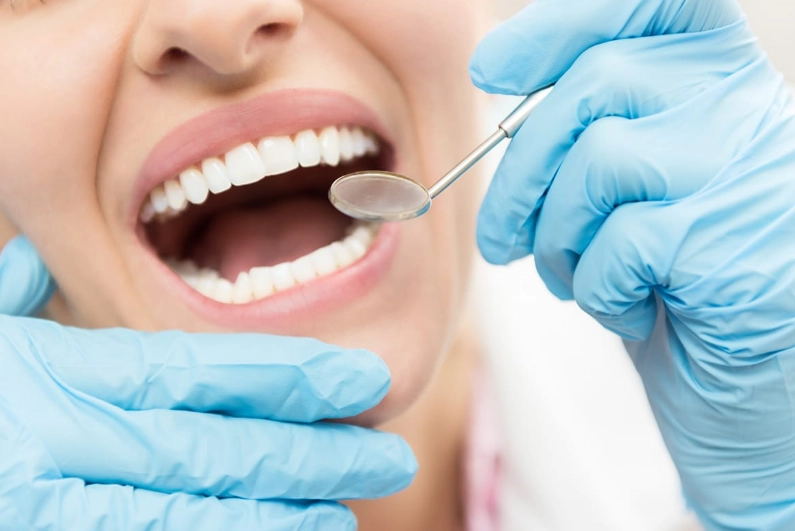
What’s Inside: Your Quick Pain Guide
The 5 Real Reasons Your Cleaning Hurts (Beyond "Sensitive Teeth")
When that ultrasonic scaler hits a tender spot, it’s usually due to one of these five culprits. Think of it as a diagnostic checklist for your discomfort.
1. Gum Inflammation (Gingivitis) – The Primary Culprit
This is the big one. Healthy gums are pink, firm, and fit snugly around your teeth. Unhealthy, inflamed gums (gingivitis) are red, swollen, and tender. The American Academy of Periodontology notes that gingivitis is caused by plaque buildup. When your hygienist cleans under your gumline, they're essentially cleaning an inflamed, open wound. It’s like having a splinter removed from a swollen finger—it’s going to be sensitive.
The subtle mistake? People often think if they don’t see blood every day, their gums are fine. But inflammation can be present without obvious bleeding. The probe used to check your gums might be the first thing that causes discomfort, tipping off your hygienist before the cleaning even starts.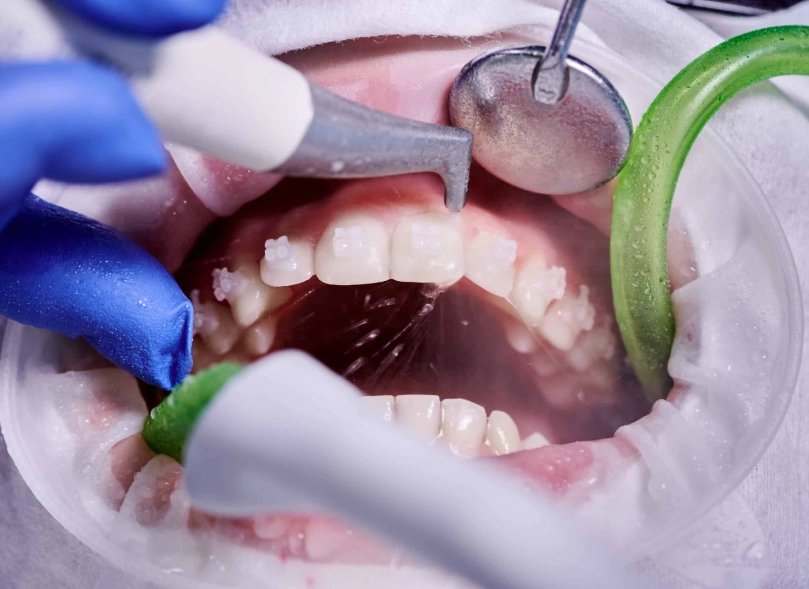
2. Tartar Buildup Below the Gumline
Tartar (calculus) is hardened plaque. When it forms above the gumline, removal is usually straightforward. The real pain comes from subgingival calculus—tartar that’s crept below the gums, attaching to the root surface. Your body sees this as a foreign object and inflames the gums around it. Removing this requires the hygienist to work in that already-inflamed pocket, which can cause a deep, sometimes sharp discomfort. The more tartar, and the deeper it is, the more likely you are to feel it.
3. Exposed Root Surfaces & Tooth Sensitivity
Gum recession, whether from brushing too hard, genetics, or past gum disease, exposes the tooth's root. The root is covered in cementum, which is softer than enamel, and contains thousands of microscopic tubules leading directly to the nerve. When cleaning tools, water, or air hit these areas, it can trigger a short, sharp pain. This isn't just "sensitive teeth" in a generic sense; it's a specific anatomical vulnerability.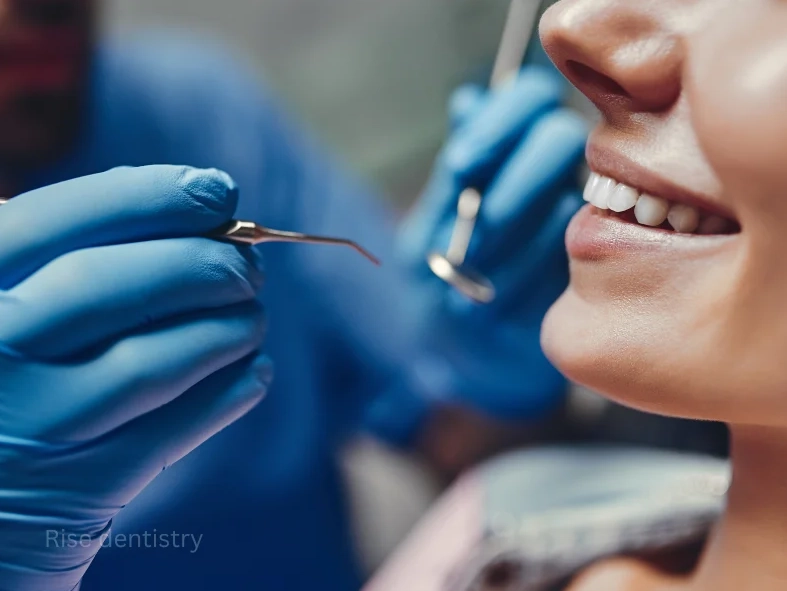
4. The Tools and The Pressure
Not all pain is biological. Some is mechanical. An ultrasonic scaler uses vibration and water to blast off tartar. The sensation can be jarring, and if the hygienist is working on a sensitive area or using a high power setting, it can hurt. Similarly, hand scalers require tactile skill. A less experienced or hurried hygienist might apply more lateral pressure than necessary. I recall one cleaning where a new hygienist seemed to be using my tooth as a fulcrum, creating a dull, aching pressure. A gentle request to ease up made a world of difference.
5. Dental Anxiety and Tension
This isn't "all in your head" in a dismissive way. It's a real physiological amplifier. When you're anxious, you tense up—especially your jaw and neck muscles. You might also breathe shallowly. This tension can make you hypersensitive to any stimulus. Furthermore, when you're braced for pain, you're not relaxed enough for your dentist to work efficiently, which can prolong the procedure, creating a vicious cycle.
Key Takeaway: A truly pain-free cleaning on unhealthy teeth is almost a contradiction. Some discomfort is a sign that the cleaning is addressing a problem area. However, excruciating pain is not a requirement and often points to issues with inflammation control or technique.
How to Talk to Your Dentist for a Less Painful Cleaning
Communication is your most powerful tool. Don't suffer in silence. Here’s a script that goes beyond "I have sensitive teeth."
Before they start: "Hi, I've had some painful cleanings in the past, especially on my lower front teeth and back molars. I'm a bit anxious about it today. Could we use a topical numbing gel before you begin, and can you let me know before you switch to a more sensitive area?"
During the cleaning: Raise your left hand (a universal "stop" signal in many dental offices) if you feel a sharp pain. Say something specific like, "That's really sharp on that tooth, can we pause for a second?" or "The pressure on my back right molar is aching." This gives actionable feedback.
Ask about options: Inquire about air polishing (a gentler alternative to scraping for surface stains) or laser-assisted cleaning (which can be more precise and less invasive for gum therapy). These are part of the trend toward minimally invasive dentistry. Not every office has them, but asking shows you're informed.
Is Pain *After* a Cleaning Normal? Red Flags vs. Recovery
A little tenderness for 24-48 hours is standard, especially if you had significant tartar removal or gum inflammation. Your gums are healing. But there's a line.
| Normal Recovery Discomfort | Potential Red Flag Pain |
|---|---|
| Generalized gum soreness, like after a workout. | Sharp, localized pain in a single tooth that lingers. |
| Sensitivity to hot/cold for a few days. | Throbbing, constant pain or a feeling of pressure. |
| Mild aching in the jaw from keeping it open. | Visible swelling of the gums or cheek. |
| Minor bleeding when brushing gently. | Bleeding that doesn't subside within 2 days. |
Red flags could indicate an incomplete cleaning leaving debris under the gums, an accidental nick that became infected, or an unrelated problem (like a cracked tooth) exacerbated by the cleaning. Don't hesitate to call your dentist if you experience these.
The Long Game: How to Prevent Cleaning Pain for Good
The ultimate goal isn't just to survive the next cleaning, but to make the next one a breeze. This requires shifting your focus from the twice-a-year event to your daily 365-day routine.
Floss. Correctly. Not just the day before your appointment. Daily flossing disrupts the plaque biofilm between teeth, preventing it from hardening into tartar and migrating below the gumline. The difference in gum inflammation between a regular flosser and a non-flosser is stark and immediately apparent to your hygienist.
Consider an Electric Toothbrush with a Pressure Sensor. It ensures you're not scrubbing your gums away, which prevents recession and root exposure. Models from Oral-B or Sonicare are clinically proven to reduce gingivitis more effectively than manual brushing.
Use a Sensitivity Toothpaste Consistently. Products with potassium nitrate or stannous fluoride (like Sensodyne or Colgate Sensitive) need 2-4 weeks of regular use to effectively block those tubules in exposed roots. Using it only when your teeth hurt is like taking a painkiller after the injury—it's reactive, not preventive.
Don't Skip Cleanings. It sounds counterintuitive, but delaying cleanings because you're afraid of pain guarantees more tartar buildup, deeper inflammation, and a more painful experience next time. Breaking that cycle requires facing it on a regular, 6-month schedule.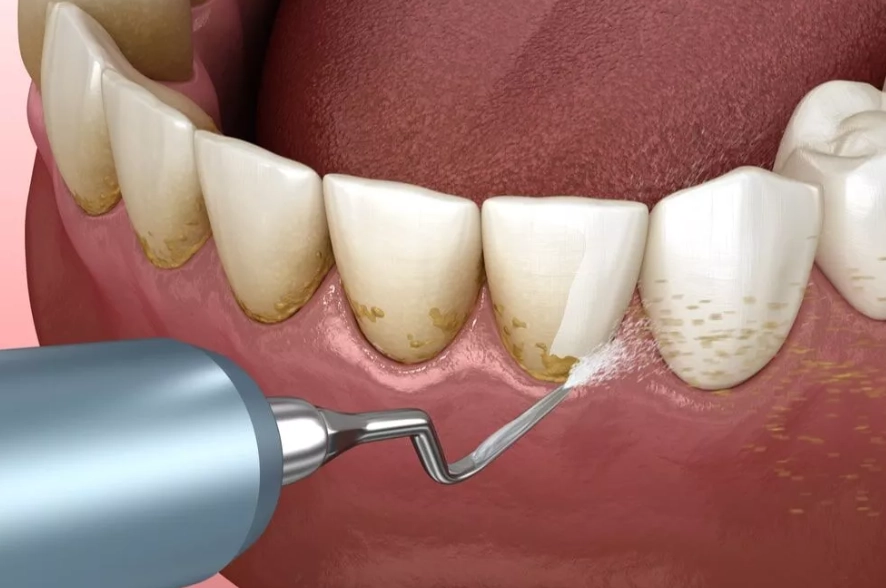
Clearing the Confusion: Your Top Cleaning Pain Questions

 The bottom line is this: pain during a dental cleaning is a message, not a life sentence. Decoding that message—whether it's about gum health, technique, or anxiety—gives you the power to change the conversation with your dental team and transform your experience from something to dread into a routine part of staying healthy.
The bottom line is this: pain during a dental cleaning is a message, not a life sentence. Decoding that message—whether it's about gum health, technique, or anxiety—gives you the power to change the conversation with your dental team and transform your experience from something to dread into a routine part of staying healthy.