You just got through a root canal. The worst of the dental pain is over, but a few days later, a new, familiar nuisance pops up: a painful canker sore on your gum, cheek, or tongue. Your mind immediately connects the dots. "Did the root canal cause this?" It's a logical question, and one I've heard countless times in my practice.
Let's cut to the chase. A root canal procedure, in its standard, successful form, does not directly create a canker sore. The bacteria and inflammatory processes involved in a root canal infection are different from the mechanism behind canker sores (aphthous ulcers). However—and this is the crucial part—the events surrounding the root canal can absolutely act as a powerful trigger for someone prone to them. It's less about the procedure itself and more about the physical and emotional fallout.
In This Article, You'll Discover:
Direct Cause or Indirect Trigger? Understanding the Mechanism
This is where most online explanations fall short. They give a simple "yes" or "no" without explaining the why. To understand, you need to know what a canker sore is. It's not a viral infection like a cold sore. The American Academy of Oral Medicine defines recurrent aphthous stomatitis (the medical term) as a complex, immune-mediated reaction. Think of it like your mouth's immune system overreacting to a perceived threat.
A root canal doesn't inject a "canker sore virus." Instead, it creates a perfect storm of conditions that can flip the switch if you're genetically predisposed. The table below breaks down this critical difference.
| Factor | Direct Cause (Not Typically from Root Canal) | Indirect Trigger (Very Possible from Root Canal) |
|---|---|---|
| Mechanism | Introduction of a specific pathogen (e.g., herpes virus). | Physical trauma, stress, or immune disruption that activates a pre-existing tendency. |
| Timing | Would occur in almost everyone undergoing the procedure. | Only occurs in individuals already prone to canker sores. |
| Analogy | Getting the flu from someone who sneezed on you. | Having a migraine triggered by lack of sleep and bright lights—you were prone to migraines, the situation set it off. |
So, if you're someone who gets canker sores from time to time, a root canal is a major event that can easily be the "bright light and lack of sleep" for your mouth.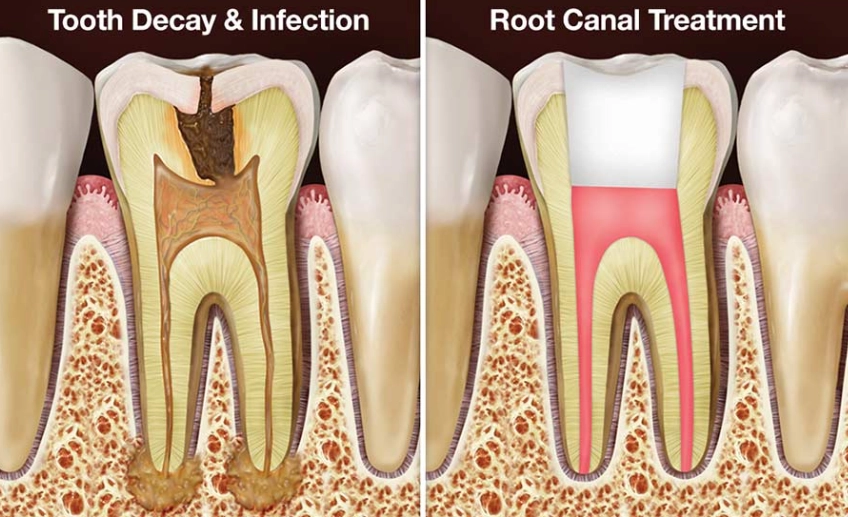
The Top 3 Ways a Root Canal Can Trigger a Canker Sore
Based on patient histories, these are the most common pathways. It's rarely just one.
1. The Unavoidable Physical Trauma
This is the biggest culprit. A root canal isn't a gentle process. Your cheek is stretched, your mouth is held open, and dental instruments—no matter how skilled the dentist—press against the soft tissues. A slip of a suction tip, the edge of a dental dam clamp, or even prolonged pressure from a finger rest can cause a small abrasion.
For most people, this heals uneventfully. For canker-sore-prone individuals, that tiny injury is a beacon for the immune system to launch an overzealous attack, resulting in the characteristic painful white or yellow ulcer with a red halo. It often appears 2-3 days post-procedure, just when you think you're in the clear.
2. The Stress Factor (It's Not Just in Your Head)
Let's be honest: few people look forward to a root canal. The anxiety, the cost, the disruption—it's significant stress. Research, including studies referenced by institutions like the Mayo Clinic, consistently links emotional stress to canker sore outbreaks. Stress hormones like cortisol can modulate immune function, making you more susceptible.
The stress doesn't end when you leave the chair. Worrying about the procedure's success, managing post-op discomfort, and the hassle of follow-ups keep your system on alert. This prolonged stress state is a classic trigger.
3. The Post-Procedure "Hygiene Overcorrection"
Here's a subtle mistake I see all the time. After a dental procedure, patients become hyper-vigilant. They brush more aggressively around the treated area to "keep it clean," fearing infection. Or, they might start using a new, harsh alcohol-based mouthwash they bought just for the occasion.
This overzealous hygiene is counterproductive. Aggressive brushing causes micro-trauma. Harsh mouthwashes (especially those with sodium lauryl sulfate, a common foaming agent) strip the delicate oral mucosa, making it more vulnerable to ulcer formation. You're trying to protect the site but inadvertently creating the conditions for a different problem.
Key Insight: If you get a sore directly opposite the tooth that was treated, on the cheek or tongue, it's almost certainly from trauma during the procedure. The soft tissue was pressed against a sharp tooth edge or an instrument during the long appointment.
Is It a Canker Sore or Something Else? A Quick Guide
Not every mouth sore after a root canal is a simple canker sore. It's vital to know the difference. A true canker sore:
- Appears inside the mouth (on movable mucosa like cheeks, lips, tongue, floor of mouth, soft palate).
- Is not contagious.
- Starts as a red bump, then forms a white/yellow center with a red border.
- Is painful, especially to spicy or acidic foods.
You should contact your dentist immediately if the "sore" has these characteristics, as it could signal a complication:
- Located on the gums directly adjacent to the treated tooth: This could be a draining abscess sinus tract or a gum infection, not a canker sore.
- Has a fever, pus, or significant swelling: Signs of a bacterial infection.
- Is on the outer lips: This is more likely a cold sore (herpes simplex), which is contagious and treated differently.
- Doesn't heal within 10-14 days: Any ulcer that persists needs professional evaluation to rule out other causes.
When in doubt, send a photo to your dentist or schedule a quick check. It's always better to be sure.
Soothing the Pain and Preventing the Next One
If you have a post-root canal canker sore, the goal is to manage pain and support healing. Forget the internet myths like applying salt directly (that just hurts more).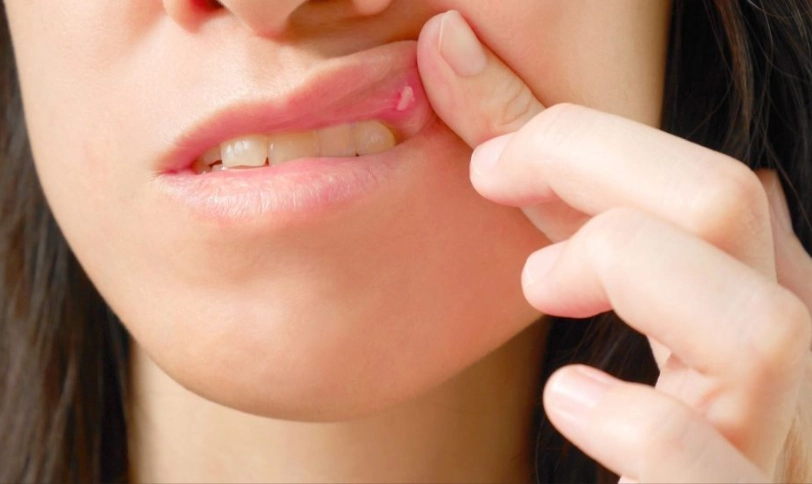
For Immediate Relief & Healing:
- Over-the-counter gels: Products with benzocaine or fluocinonide can numb the area and protect it. Apply a small dab after meals and before bed.
- Gentle mouth rinses: Use a warm saltwater rinse (1/2 tsp salt in 1 cup warm water) or a baking soda rinse. Swish gently for 30 seconds, 2-3 times a day. This soothes and cleans without harsh chemicals.
- Diet tweaks: Avoid the "triple threat": acidic foods (citrus, tomatoes), sharp foods (chips, toast crusts), and spicy foods. Stick to soft, bland foods like yogurt, mashed potatoes, and smoothies until it heals.
- Protect the area: If it's near a sharp tooth edge, ask your dentist about temporary dental wax to create a smooth barrier.
To Prevent a Repeat Performance After Future Dental Work:
- Talk to your dentist beforehand: Say, "I'm very prone to canker sores. Can we be extra mindful of soft tissue during the procedure?" A good dentist will use additional cushioning and check in on your comfort.
- Post-op hygiene, done right: Brush the treated area gently with an ultra-soft toothbrush. Avoid alcohol-based mouthwashes. Stick to your usual gentle rinse or saltwater.
- Manage stress proactively: This might mean deep breathing before and after the appointment, scheduling it at a low-stress time, or even discussing anti-anxiety options with your dentist if your fear is severe.
- Consider a preventative supplement: Some studies suggest that regular sufferers may benefit from B-vitamin complex, lysine, or zinc supplements. Discuss this with your doctor or dentist to see if it's right for you.
Your Questions, Answered (Beyond the Basics)
 I've never had a canker sore before in my life. Is it likely my root canal caused this first-ever one?
I've never had a canker sore before in my life. Is it likely my root canal caused this first-ever one?The bottom line is this: while a root canal isn't a direct cause of canker sores, it's a masterclass in triggering them. By understanding the link—physical trauma, stress, and hygiene changes—you can take proactive steps to minimize your risk and handle any sores that do appear with confidence, knowing it's a common, manageable side effect of a major dental intervention, not a sign that something went wrong with the procedure itself.