Let's be honest, the words "root canal" can make anyone nervous. But here's the thing most dental blogs gloss over: the procedure itself is often the easy part, thanks to modern anesthesia. The real mystery, and source of anxiety, is what happens after. How long will I be out of commission? When can I eat a proper meal again? Is this level of pain normal on day three? I've seen patients breeze through recovery and others hit unexpected bumps, and the difference usually comes down to managing expectations and knowing a few key tricks. This guide cuts through the generic advice to give you a clear, day-by-day breakdown of root canal recovery time and the practical steps you can take to influence it.
What's Inside This Guide
What is the Typical Root Canal Recovery Timeline?
Forget the vague "a few days" answer. Recovery isn't a single event; it's a process with distinct phases. The initial, most sensitive healing of the gums and ligament around the tooth takes about 3 to 7 days. However, the bone at the tip of the root, which was also irritated by the infection, continues to remodel and heal for several months. You won't feel this deeper healing, but it's why your dentist might wait before placing the final crown.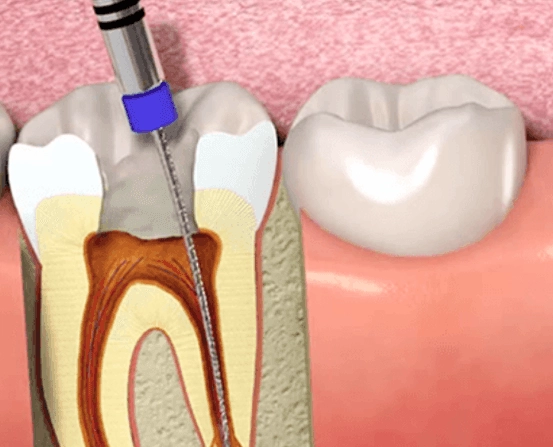
Here’s a more useful breakdown of what you can realistically expect in the first week:
| Time Frame | What You'll Likely Feel | What You Can (and Can't) Do |
|---|---|---|
| First 24-48 Hours | Numbness wearing off, followed by moderate soreness or throbbing. Peak discomfort is usually within the first 12 hours. | Stick to soft, cool foods. Rest. Avoid chewing on that side entirely. Take prescribed or OTC pain meds as directed before numbness fully wears off. |
| Days 3-5 | Significant improvement. Soreness changes from a persistent throb to a dull ache only when you press on the tooth or chew something slightly firm. | You can gradually reintroduce semi-soft foods. You can likely return to most normal non-strenuous activities. Gentle brushing around the area is okay. |
| Days 6-7+ | Minimal to no discomfort. The tooth and gum should feel mostly normal. | You can usually resume a normal diet, but still be cautious with extremely hard foods (nuts, hard candy) until the permanent crown is placed. Most people feel fine returning to work and exercise. |
A huge factor people don't consider is the starting condition of your tooth. If you had a massive infection and swelling before the procedure (what dentists call an "acute apical abscess"), your body has more inflammation to resolve. Your recovery might lean toward the 7-day mark or even a bit longer. A routine root canal on a tooth that wasn't actively painful? You might feel great in 2-3 days.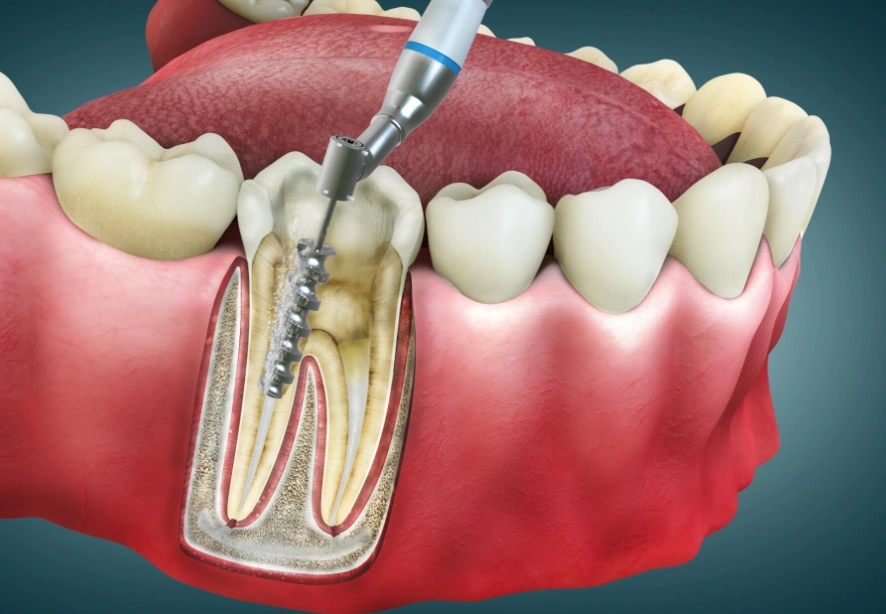
A Closer Look at Activity Milestones
Let's get specific about common concerns.
Returning to Work: If you have a desk job, you can probably go back the next day, armed with some ibuprofen. For physically demanding jobs (construction, nursing with lots of lifting), I'd recommend taking 2-3 days off. The strain can increase throbbing.
Exercise: Light walking is fine immediately. Hold off on heavy weightlifting, high-impact cardio, or hot yoga for at least 3-4 days. The increased blood pressure and heart rate can trigger post-operative pain. I've had more than one patient call me after a tough gym session on day two wondering why the pain came back with a vengeance.
Eating: This is where people get into trouble. The temporary filling is just that—temporary. It's not designed for massive force.
- Days 1-2: Yogurt, smoothies (no straw!), mashed potatoes, soup (lukewarm), applesauce, pudding.
- Days 3-5: Scrambled eggs, pasta, soft fish, oatmeal, well-cooked vegetables.
- Day 7+: You can be more adventurous, but treat the tooth like it's wearing a protective helmet that's not superglued on. Avoid sticky caramel and tearing into a hard baguette.
Managing Pain and Discomfort: A Realistic Approach
You will have some discomfort. Accepting that reduces panic. The goal isn't zero pain; it's manageable pain that steadily decreases.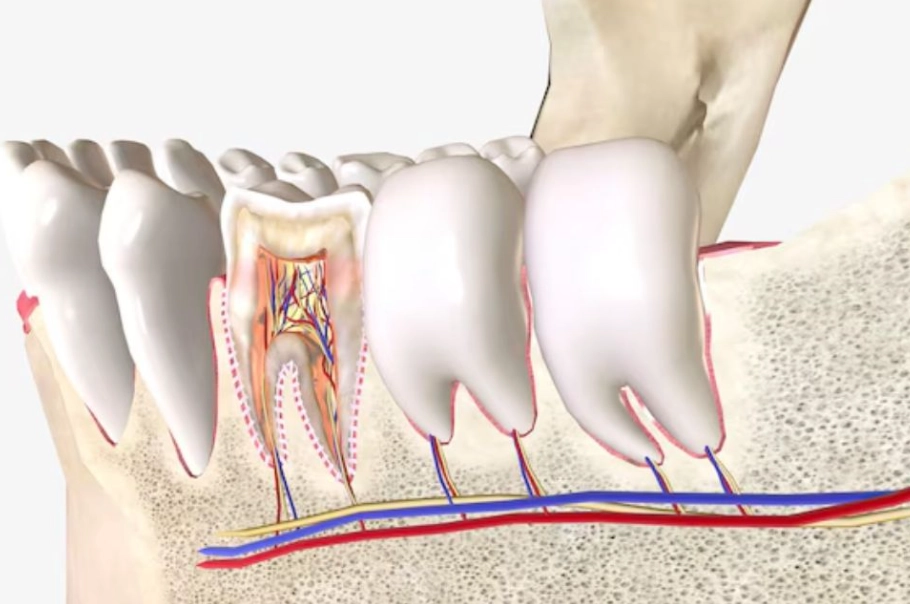
The most effective strategy is a pre-emptive and layered approach to medication, not a reactive one. If your dentist prescribes an antibiotic, finish the entire course, even if you feel better. The infection is the primary cause of long-term pain, not the procedure.
Medication Tip: A common and effective regimen is alternating ibuprofen (Advil) and acetaminophen (Tylenol). They work through different pathways. For example, take ibuprofen, then 3 hours later take acetaminophen, then 3 hours later ibuprofen again. This creates a steady coverage. Always confirm this schedule with your dentist or doctor first, especially if you have underlying health conditions.
Cold compresses are your best friend for the first 36 hours. Apply an ice pack wrapped in a thin towel to the outside of your cheek in cycles: 15 minutes on, 15 minutes off. This reduces swelling and numbs the area. After about 48 hours, if there's still swelling, some dentists suggest switching to gentle warmth to increase blood flow and promote healing—but when in doubt, ask yours.
Sleep propped up with an extra pillow for the first night or two. Keeping your head elevated reduces pressure in the blood vessels around the tooth, minimizing that pounding sensation.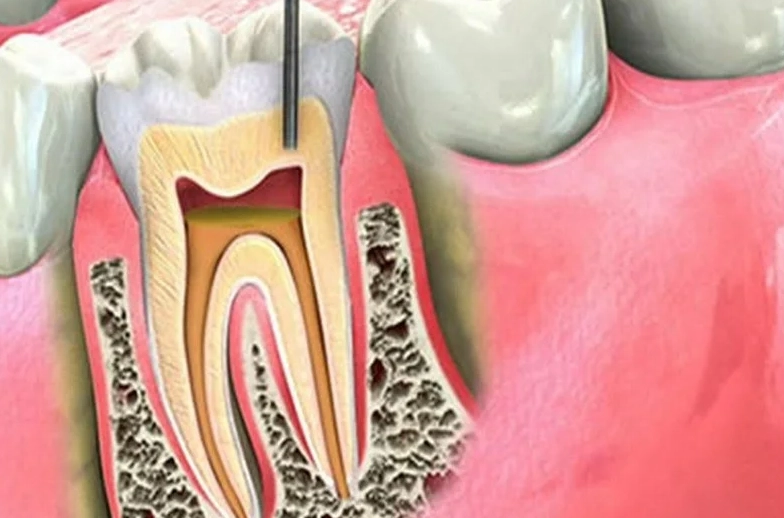
How to Heal Faster: Tips Most Patients Miss
Here's where you can actively improve your recovery timeline. These aren't just generic "rest well" tips.
Nutrition is Medicine: In the first few days, focus on foods high in protein (Greek yogurt, protein shakes) and vitamin C (blended berries in a smoothie). Your body needs raw materials to repair tissue. Avoid sugary foods and drinks—they feed any residual bacteria and promote inflammation. Stay hydrated with water.
The Oral Hygiene Balancing Act: Yes, brush and floss. But on the treated side, be gentle. Use a soft-bristled brush and don't aggressively scrub the gum line around the tooth. You can gently rinse with warm salt water (1/2 teaspoon salt in a cup of warm water) after meals starting the day after the procedure. This soothes gums and keeps the area clean. Avoid commercial alcohol-based mouthwashes for the first week; they can be irritating.
The Biggest Mistake: Using the treated tooth to "test" if it's better. On day four, feeling pretty good, you think, "Let me just try a pretzel." Don't. You'll set yourself back. Let pain be your guide, not curiosity.
Smoking and Alcohol: Just don't. Smoking drastically reduces blood flow, starving the healing tissues of oxygen and nutrients. It's a guaranteed way to prolong pain and increase the risk of a dry socket-like pain in the bone (rare but possible after root canals). Alcohol can interact with medications and dehydrate you.
Red Flags: When to Call Your Dentist
Most recoveries are straightforward. But know the signs that something's off. Call your dentist if you experience:
- Severe, escalating pain that isn't controlled by your prescribed medication after 2-3 days.
- Visible, increasing swelling in your cheek, jaw, or under your tongue that gets worse after 48 hours.
- A bad taste or pus coming from the tooth, or a fever over 100.4°F (38°C).
- The temporary filling falls out completely and isn't replaced promptly (this exposes the inside of the tooth to saliva and bacteria).
- Pain that feels like a sharp, electric shock or significant pain when you bite down after the first week has passed.
Trust your instinct. If something feels wrong, it's better to get it checked. A quick follow-up visit can often resolve a minor issue before it becomes a major problem.
Your Root Canal Recovery Questions Answered
Is it normal to have jaw soreness after a root canal, and how long does that last?
Absolutely normal, and it's one of the most common complaints that surprises patients. You've had your mouth open wide, sometimes for over an hour, and the dentist or endodontist has applied pressure. This strains the temporomandibular joint (TMJ) and muscles. This jaw muscle soreness often feels like a dull ache and can last 3-5 days, sometimes outlasting the tooth pain itself. Gentle jaw stretches, warm compresses on the joint (not the tooth after 48 hours), and soft foods help.
My root canal recovery time seems much longer than my friend's. Why is that?
Comparing recoveries is a surefire way to worry unnecessarily. Several variables are at play: the complexity of your root anatomy (some teeth have tiny, curved canals that are harder to treat), the size of the pre-existing infection, your own immune system's inflammatory response, and even how meticulously you follow the aftercare instructions. A molar root canal is typically a bigger ordeal than a front tooth root canal. Your timeline is your own.
Can I drive myself home after the procedure?
If you only had local anesthesia (the standard numbing shots), yes, you can drive. You are numb, not sedated. However, if you opted for oral sedation or nitrous oxide (laughing gas) to manage anxiety, you will need a driver. Always clarify this with your dental office before your appointment.
When is it safe to drink from a straw after a root canal?
class="item-answer">Wait at least 5-7 days. The suction created in your mouth when using a straw can dislodge the blood clot that's forming in the deep tissues around the root tip, a condition similar to a "dry socket" that can be very painful. It's an easily avoidable risk. Just sip normally from a cup.How soon after a root canal can I get the permanent crown?
Most dentists prefer to wait 2-4 weeks. This waiting period allows for the significant initial inflammation inside the bone to subside. Taking the final impression for a crown too soon, while the gums are still slightly swollen, can result in a crown that doesn't fit perfectly once everything settles. A poorly fitted crown is a leading cause of post-root canal failure.