Let's cut straight to the point. The idea of killing a tooth pain nerve in 3 seconds permanently is a dramatic oversimplification, often found in alarming online videos and forums. It sells a fantasy of instant, pain-free resolution. The biological reality? It's impossible. However, modern dentistry does have procedures that can permanently remove an infected or damaged tooth nerve, ending the pain for good. The process isn't measured in seconds, but in a careful, professional appointment. If you're searching for this phrase, you're likely in serious pain and desperate for a real solution. This guide will dismantle the myths, explain what actually works, and walk you through the only proven path to permanent relief.
What’s Inside This Guide
Is It Possible to Kill a Tooth Nerve in 3 Seconds?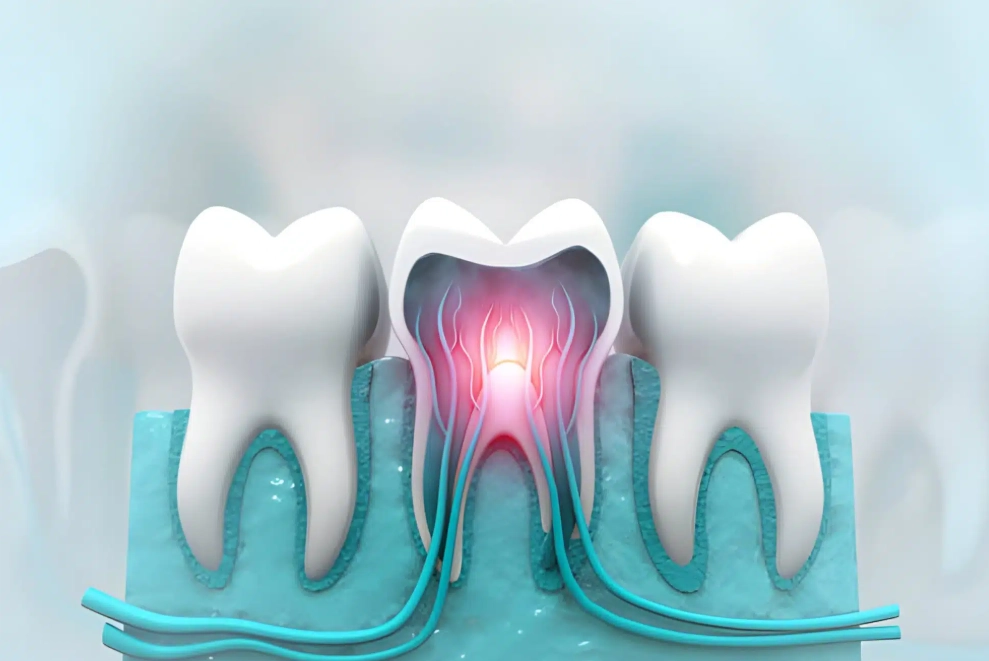
No. Absolutely not. Think about what the nerve is—a bundle of living tissue and blood vessels (the dental pulp) deep inside the hard shell of your tooth. To access it, a dentist needs to drill through enamel and dentin. That alone takes longer than three seconds with local anesthesia. Then, the nerve tissue must be meticulously cleaned out and the space disinfected. Any claim of a three-second permanent fix is either referring to a dangerous, non-sterile DIY method or is pure clickbait.
I've seen patients who tried these "quick fixes"—applying aspirin directly to the gum, using super-strong alcohol, or even attempting to poke the tooth with a pin. The result is never a cured tooth. It's usually a worsened infection, chemical burns on the gums, or simply a masked pain that returns with a vengeance as the underlying decay reaches the nerve. The American Dental Association (ADA) strongly warns against any form of self-treatment for a toothache, as it can lead to serious complications.
What's Actually Causing Your Tooth Nerve Pain?
To understand the solution, you need to know the problem. That throbbing, sharp, or lingering pain is a signal. Your tooth's nerve is under attack, usually by one of these culprits:
- Deep Decay (Cavities): Bacteria eat through the enamel and dentin, finally reaching the pulp chamber. This is the most common cause.
- Cracked or Fractured Tooth: A crack can provide a pathway for bacteria to infect the pulp, or it can physically irritate the nerve.
- Trauma: A blow to the tooth can damage the blood supply to the nerve, causing it to die slowly (a process called pulp necrosis).
- Severe Gum Disease: In advanced stages, infection from the gums can travel up through the tooth's roots to affect the nerve.
The pain often follows a pattern. It might start as sensitivity to hot, cold, or sweets. Then it progresses to a spontaneous, throbbing ache that might even wake you up at night. Once the nerve is irreversibly inflamed or dead, the pain can become constant and severe. The goal of treatment isn't just to "kill" the nerve—it's to remove the entire infected or necrotic pulp tissue and seal the tooth to prevent re-infection.
How Does a Dentist Actually Remove a Tooth Nerve Permanently?
The gold-standard procedure is a root canal treatment (endodontic therapy). Forget the horror stories; with modern techniques and anesthesia, it's typically no more uncomfortable than getting a deep filling. Here’s what the process really looks like, step by step, based on my own experience performing them.
- Diagnosis and X-ray: The dentist confirms the tooth is the source and takes an X-ray to see the shape of the roots and the extent of infection.
- Local Anesthesia: The area is completely numbed. You should feel pressure, not pain.
- Access Opening: A small opening is made in the top of the tooth to reach the pulp chamber.
- Cleaning and Shaping: Using tiny instruments, the dentist removes the diseased pulp, cleans, disinfects, and shapes the root canals. This is the most time-consuming part, ensuring all infected material is gone.
- Filling: The now-empty, clean canals are filled with a biocompatible material (usually gutta-percha) to seal them.
- Restoration: The access hole is sealed with a temporary or permanent filling. Often, a crown is recommended later to protect the now-weakened tooth.
The entire procedure for a single-rooted tooth might take 30-60 minutes. A molar with multiple roots can take 90 minutes or more. This is the definitive, permanent solution. The nerve is gone, and the pain source is eliminated.
| Procedure | What It Does | Is It Permanent? | Typical Duration & Notes |
|---|---|---|---|
| Root Canal Therapy | Removes infected pulp, cleans/seals canal | Yes, with proper restoration | 60-90 min. Success rate >95% (American Association of Endodontists). |
| Tooth Extraction | Removes the entire tooth, including nerve | Yes (tooth is gone) | 20-40 min. Permanent solution but creates a gap needing replacement (implant, bridge). |
| Pulp Capping (Indirect/Direct) | Attempts to save a minimally exposed/inflamed pulp | Not always; may delay root canal | Quick procedure. Only works if pulp isn't severely infected. |
| Over-the-Counter Painkillers | Reduces inflammation & pain signals | No. Temporary mask. | Effects last 4-8 hours. Does not address the cause. |
Cost is a real concern. A root canal on a front tooth can range from $700 to $1,200, while a molar might be $1,000 to $1,800 or more, depending on location and complexity. Dental insurance often covers 50-80% of endodontic procedures. An extraction is cheaper upfront ($150-$400) but the cost of replacing the tooth later is much higher.
Managing the Pain at Home Before Your Appointment
You have a dental appointment scheduled, but you need to survive the night. Here are practical, safe strategies that actually help manage the pain temporarily. None of these "kill" the nerve, but they can make you more comfortable.
- Cold Compress: Apply a cold pack wrapped in a thin cloth to the outside of your cheek for 15-minute intervals. This reduces inflammation and numbs the area.
- Elevate Your Head: When sleeping or resting, use an extra pillow. This can reduce the throbbing pressure in the area.
- Salt Water Rinse: Dissolve half a teaspoon of salt in a glass of warm water. Swish gently for 30 seconds. This helps cleanse the area and reduce gum inflammation around the tooth.
- Clove Oil (Use with Caution): Clove oil contains eugenol, a natural anesthetic. Dip a cotton ball in water, then add a tiny drop of clove oil. Dab it only on the gum around the painful tooth, not inside the cavity. It can irritate soft tissues, so this is a last-resort, spot-treatment.
- Avoid Triggers: Stay away from extremely hot, cold, sweet, or hard foods that will aggravate the exposed nerve.
Signs You Can't Wait Any Longer to See a Dentist
Home care is a temporary bridge, not a destination. Certain symptoms mean the infection is spreading and you need urgent professional care. Don't gamble with these.
If you have severe, constant pain that painkillers barely touch, that's a major red flag. Swelling in your cheek, jaw, or gums near the tooth is a sign of a spreading abscess. A fever accompanying the toothache means your body is fighting a systemic infection. A bad taste in your mouth or pus draining from around the tooth is a clear indicator of an abscess that needs drainage and antibiotics.
I once had a patient who waited two weeks with a swollen cheek, trying every home remedy. By the time he came in, the infection had created a sinus tract and required emergency treatment and a strong course of antibiotics. The root canal was more complex and the recovery longer. Acting early almost always leads to a simpler, cheaper, and less painful outcome.
Your Top Questions on Tooth Nerve Pain, Answered
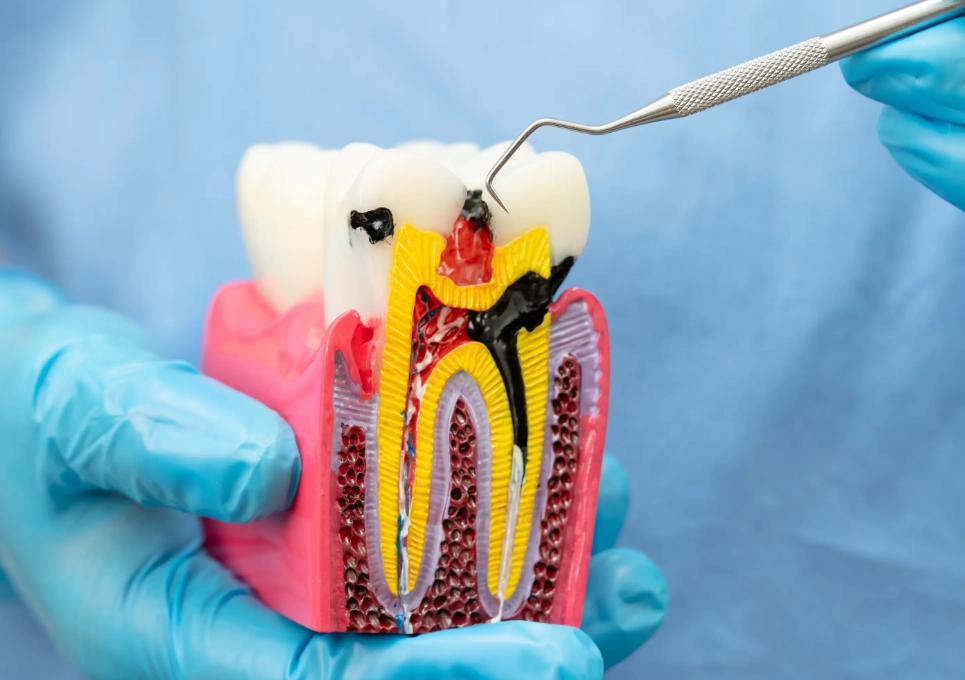 Is extraction always a cheaper and easier alternative to a root canal?
Is extraction always a cheaper and easier alternative to a root canal?