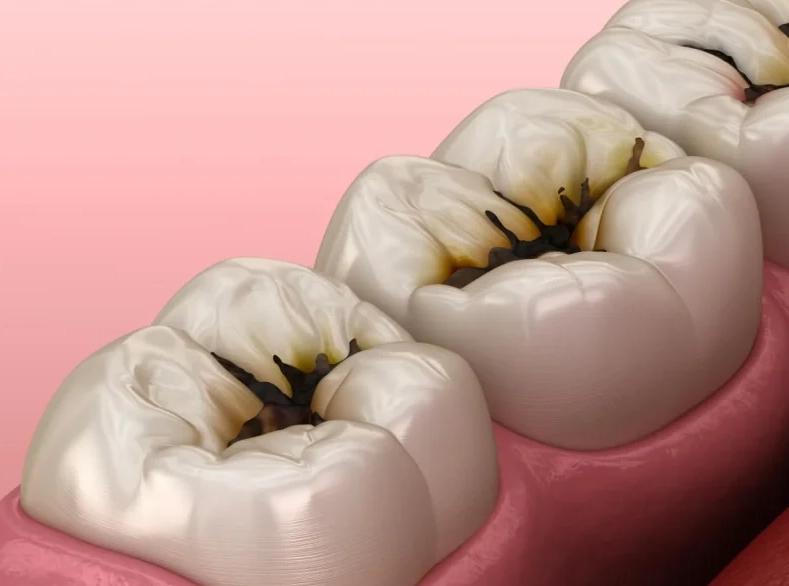
Let's cut to the chase. The phrase "root canal" sends a shiver down most people's spines, but the procedure itself is a hero, not a villain. It's the last-ditch effort to save a tooth that's under attack from the inside. The real villain is the infection or damage deep within your tooth's pulp—the soft tissue housing nerves and blood vessels.
I've seen patients panic at the mere suggestion of one. But understanding what causes a root canal demystifies it. It's not a random punishment; it's a specific response to a specific dental crisis. Think of it like a surgeon removing an inflamed appendix to save the patient. The root canal treatment removes the infected pulp to save your tooth.
Here's What We'll Cover
What's Actually Inside Your Tooth? (It's Not Just Hard Stuff)
Underneath the hard enamel and dentin layers lies the pulp chamber. This isn't just empty space. It's living tissue—nerves, blood vessels, and connective tissue. Its job is to nourish the tooth during development. Once the tooth is fully grown, the pulp's role diminishes, but if it gets infected or damaged, the problems start.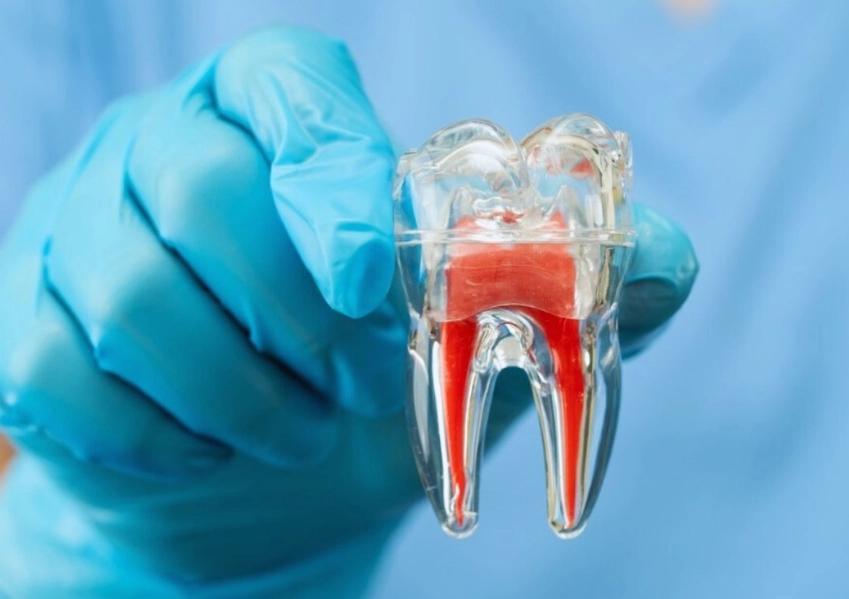
Infected pulp doesn't get better on its own.
Bacteria multiply, the infection spreads, and eventually, it can work its way out the tip of the root into your jawbone. That's when you get a painful abscess. A root canal stops this entire chain reaction by removing the source: the diseased pulp.
The 4 Main Culprits Behind Needing a Root Canal
It usually boils down to one of these four scenarios. In my practice, deep tooth decay is the most common offender, but the others are frequent visitors too.
| Cause | How It Happens | A Key Detail Most Miss |
|---|---|---|
| Deep Decay (Cavities) | Untreated cavities act like a highway for bacteria. They tunnel through enamel, then dentin, and finally breach the pulp chamber. | A small cavity on the surface can hide a massive destruction underneath. X-rays often reveal the true, alarming extent. |
| Cracked or Chipped Tooth | A crack can provide a direct pathway for bacteria to reach the pulp. Even a hairline fracture, invisible to the eye, can be enough. | Teeth grinding (bruxism) is a silent crack creator. You might not feel the grinding, but your teeth bear the stress microfractures. |
| Repeated Dental Procedures | Multiple large fillings or procedures on the same tooth can eventually irritate or inflame the pulp over time. | The pulp isn't infinitely resilient. Each procedure adds cumulative stress, sometimes leading to a slow, silent necrosis (death) of the pulp. |
| Trauma or Injury | A blow to the mouth can damage the pulp's blood supply, causing it to die even if the tooth looks intact. | This can happen months or even years after the initial injury. The tooth may darken in color, a telltale sign of internal damage. |
From the Chairside: I once had a patient, let's call him Mark, who had a "tiny" cavity filled years ago. He skipped check-ups. When he finally came in with mild sensitivity, the X-ray showed the decay had spread under the old filling like a shadow, reaching the nerve. The lesson? That minor cavity was a ticking time bomb. Regular check-ups aren't just cleanings; they're surveillance missions.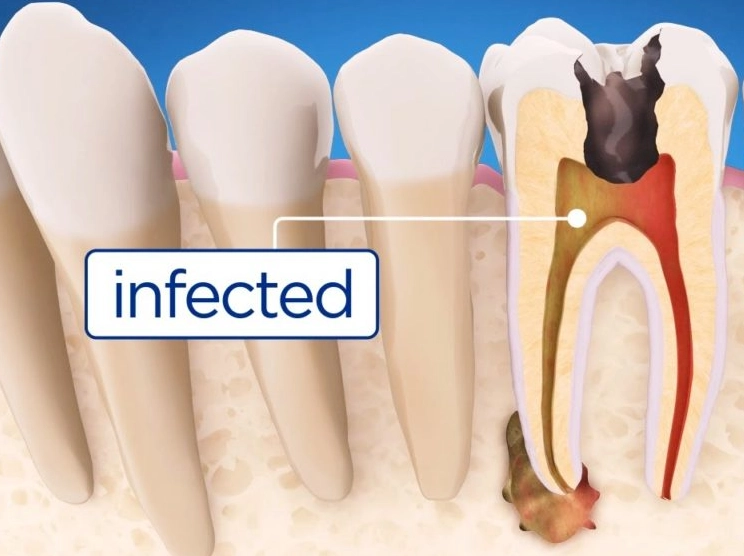
Symptoms You Can't Afford to Ignore
Sometimes the signs are dramatic, sometimes subtle. Here’s what to watch for:
- Persistent Toothache: Pain that lingers, especially when chewing or applying pressure. It might throb or be constant.
- Prolonged Sensitivity: Sharp pain with hot or cold foods/drinks that continues long after the stimulus is gone.
- Tooth Discoloration: A graying or darkening of the tooth, often from internal tissue breakdown.
- Swollen, Tender Gums: Swelling near the affected tooth, sometimes with a pimple-like bump (a sinus tract) on the gums.
- A Feeling of "Elevation": The tooth might feel slightly taller than the others when you bite down.
Here's the tricky part.
Sometimes, there are no symptoms at all. The pulp dies quietly, and the problem is only spotted on a routine X-ray. This is why skipping dental check-ups is such a gamble.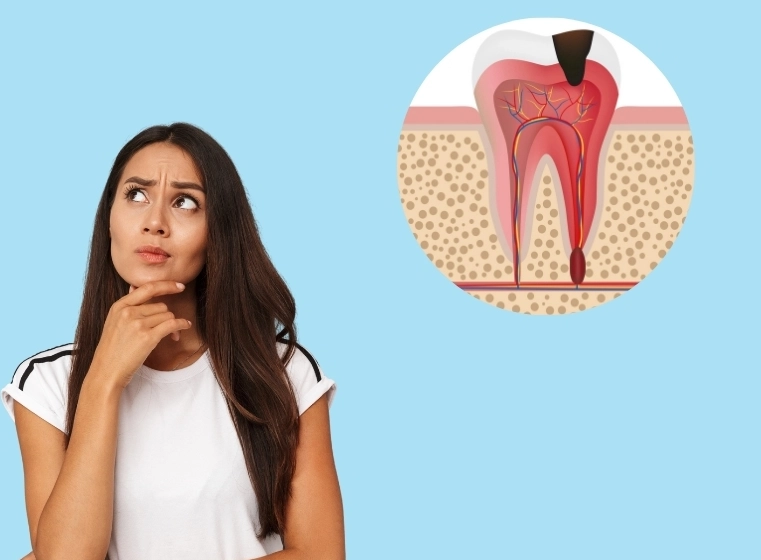
How Dentists Diagnose the Need for a Root Canal
We don't just guess. Diagnosis is a detective game combining several clues:
1. The Symptom Interview
I'll ask you to describe the pain. When does it start? What makes it better or worse? The pattern of pain is a huge clue.
2. Clinical Tests
This involves physically checking the tooth. I might tap on it (percussion test), apply a cold stimulus, or use an electric pulp tester to see if the nerve responds normally.
3. The Digital X-Ray (The Smoking Gun)
This is crucial. An X-ray can reveal decay reaching the pulp, changes in the bone around the root tip (indicating an infection), or a dark shadow traveling down the length of the root. According to the American Association of Endodontists, advanced 3D imaging (CBCT) is sometimes used for complex cases to see the anatomy in detail.
What the Root Canal Procedure Actually Involves
Forget the horror stories. With modern anesthesia, it's typically no more uncomfortable than getting a deep filling.
- Numbing & Isolation: The area is completely numbed. A small rubber dam is placed around the tooth to keep it clean and dry.
- Access Opening: A small opening is made in the crown of the tooth to reach the pulp chamber.
- Cleaning & Shaping: Tiny instruments are used to remove the diseased pulp, clean, disinfect, and shape the inner canals.
- Filling & Sealing: The now-empty, clean canals are filled with a biocompatible material called gutta-percha and sealed with adhesive cement.
- Restoration: The access hole is sealed with a temporary or permanent filling. Almost always, a dental crown is recommended afterward to protect the now-weakened tooth from breaking.
The whole process might take one or two appointments, depending on the tooth's complexity.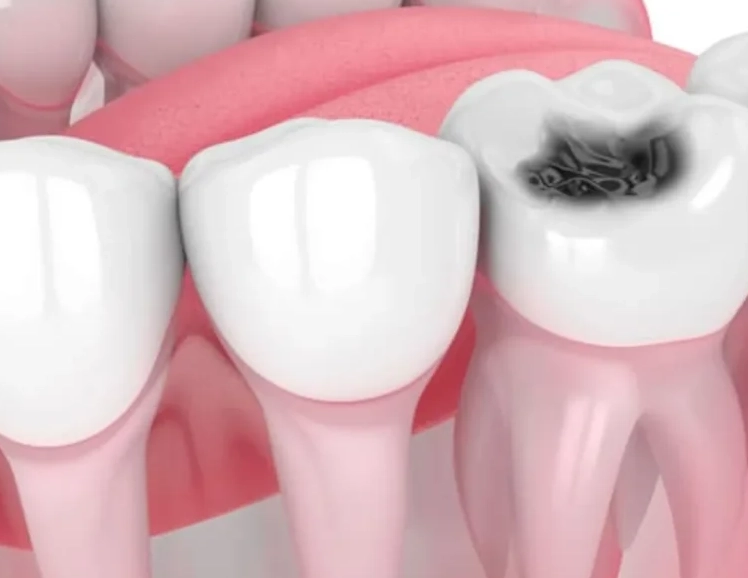
Cost Considerations & The Ultimate Goal: Prevention
Costs vary wildly by location, tooth (molars are more complex), and whether you see a general dentist or a specialist (endodontist). In the US, you might be looking at $700-$1,500 for the root canal itself from a general dentist, plus another $1,000-$2,000 for the crown. Dental insurance often covers a portion.
But the real win is avoiding it altogether. Prevention is cheaper and painless.
- Brushing & Flossing Like You Mean It: This disrupts the plaque biofilm that causes decay. Don't just scrub; angle the brush toward the gums and be thorough.
- Regular Dental Check-ups & Cleanings: Twice a year isn't a marketing ploy. It's the interval where we can catch problems when they're small and cheap to fix.
- Address Bruxism: If you grind your teeth, a nightguard is a fantastic investment to prevent cracks.
- Wear a Mouthguard for Sports: A simple, custom-fit guard can prevent traumatic injuries.
- Don't Delay Treatment: That small cavity is a $150 filling today or a $2,500 root canal and crown tomorrow. The math is simple.