Let's get straight to the point. The best time to remove wisdom teeth is typically in your late teens or early twenties, before they cause obvious problems. That's the standard advice, and for good reason—the roots aren't fully formed, and bone heals faster. But that's just the headline. The real answer to "when to remove wisdom teeth" is far more nuanced and depends entirely on your unique mouth. I've seen patients in their 50s sail through extraction because their teeth were straightforward, and 18-year-olds have a tougher time due to complex, deep impactions. This guide will walk you through the signs, the science, and the scenarios that demand action, so you can have an informed conversation with your dentist or oral surgeon.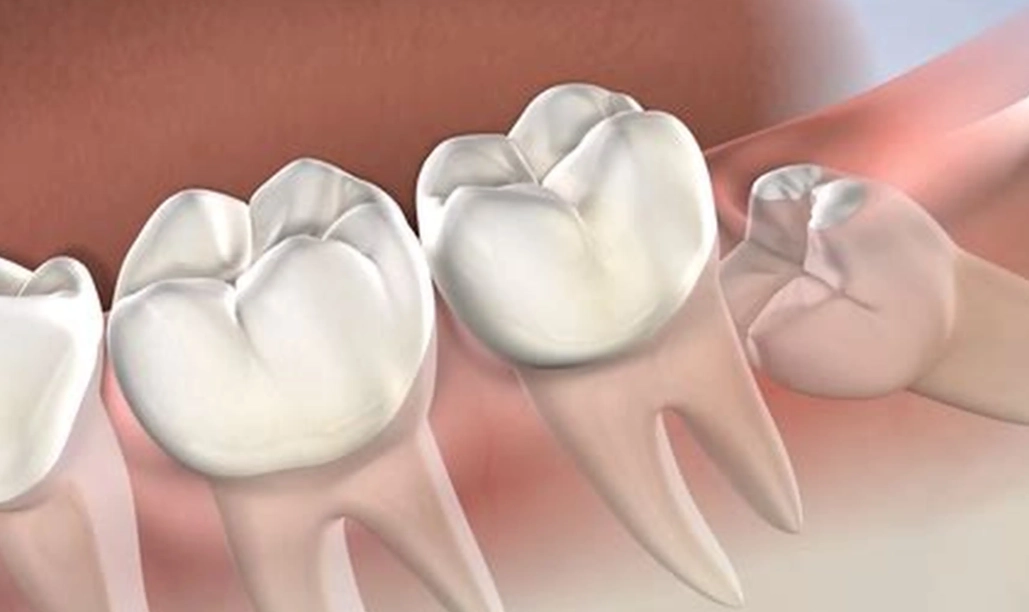
Quick Navigation: What You'll Learn
What's the Best Age to Remove Wisdom Teeth?
Most dental professionals point to the ages between 17 and 25 as the "golden window." Why? At this stage, the tooth roots are about two-thirds developed. This makes the extraction process mechanically easier for the surgeon—there's less tooth to wrestle out. More importantly, your body's regenerative capacity is near its peak. Healing is generally quicker, with less postoperative discomfort and a lower risk of complications like dry socket.
But here's a non-consensus point I stress to my patients: Your overall health and the tooth's position are more critical than your birth certificate. An older, healthy adult with a partially erupted, accessible wisdom tooth might have a simpler recovery than a younger person with a fully impacted, horizontal tooth sitting on a nerve. The American Association of Oral and Maxillofacial Surgeons (AAOMS) recommends a evaluation by the age of 25, but their guidelines emphasize condition-based decision making over age-based mandates.
Routine panoramic X-rays are the key. They're the crystal ball that shows what's brewing under the gums. Your dentist isn't just looking at the teeth themselves, but their relationship to the adjacent molars, the jawbone, and the inferior alveolar nerve (the nerve that gives feeling to your lower lip and chin).
Key Warning Signs You Need Your Wisdom Teeth Out
Sometimes, the decision is made for you. Your mouth sends clear signals. Ignoring these is like ignoring a check engine light—it usually leads to a bigger, more expensive problem down the road.
The Unmistakable Red Flags
Persistent Pain or Swelling: This is the most common driver to the surgeon's office. Throbbing pain at the back of your mouth, especially when chewing or biting down, often indicates infection (pericoronitis) or pressure.
Repeated Gum Infections: A partially erupted wisdom tooth creates a perfect trap for food and bacteria—a flap of gum tissue over part of the tooth. This leads to tender, red, swollen gums that bleed easily and can cause bad breath or a bad taste.
Damage to Other Teeth: This is a silent killer. A wisdom tooth pushing against your second molar can cause resorption (erosion) of that tooth's roots or create a cavity-prone area that's impossible to clean. I've had to perform root canals on otherwise healthy second molars because an impacted wisdom tooth destroyed the enamel on its back side.
Cysts or Tumors: Rare but serious. A fluid-filled sac (cyst) can form around an impacted tooth, destroying jawbone and potentially damaging nerves. Panoramic X-rays are crucial for detecting these early.
The Subtle (But Important) Indicators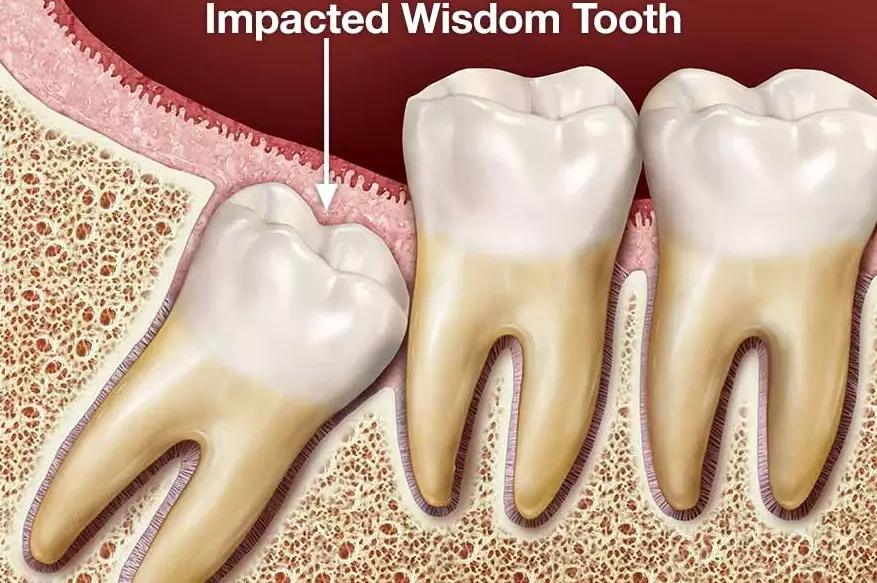
Crowding and Shifting Teeth: The debate is ongoing, but many orthodontists believe pressure from wisdom teeth can contribute to the gradual crowding of front teeth, especially after braces. If you've invested in a straight smile, protecting that investment is a valid consideration.
Headaches and Jaw Pain: While not always directly linked, problematic wisdom teeth can contribute to muscle tension in the jaw (TMJ disorders), leading to referred pain in the temples and head.
Simply Impossible to Clean: If you can't get a toothbrush or floss back there, it's not a matter of if it will get a cavity or cause gum disease, but when.
What to Expect During and After Wisdom Teeth Removal
Knowing what happens can ease a lot of anxiety. It's a routine procedure, but "routine" doesn't mean it's trivial. Here's a breakdown.
The Procedure: It's Not One-Size-Fits-All
Your experience depends heavily on the complexity of the extraction and the anesthesia chosen.
| Anesthesia Type | Best For | What You Experience | Typical Cost Influence |
|---|---|---|---|
| Local Anesthesia | Simple, fully erupted teeth. You're awake but numb. | Pressure and movement, no pain. You can drive yourself home. | Lowest cost. |
| IV Sedation (Twilight Sedation) | Most common for multiple or impacted removals. You're deeply relaxed and may sleep. | No memory of the procedure. You'll need a driver. | Adds a significant fee ($300-$800). |
| General Anesthesia | Extremely complex cases or severe patient anxiety. You are completely unconscious. | No awareness. Requires an anesthesiologist and a driver. | Highest cost addition. |
The surgeon will make an incision in the gum, remove any bone blocking access, section the tooth into pieces if necessary, extract it, clean the site, and suture it closed. The whole process for all four teeth often takes under an hour.
The Recovery Timeline: A Realistic Look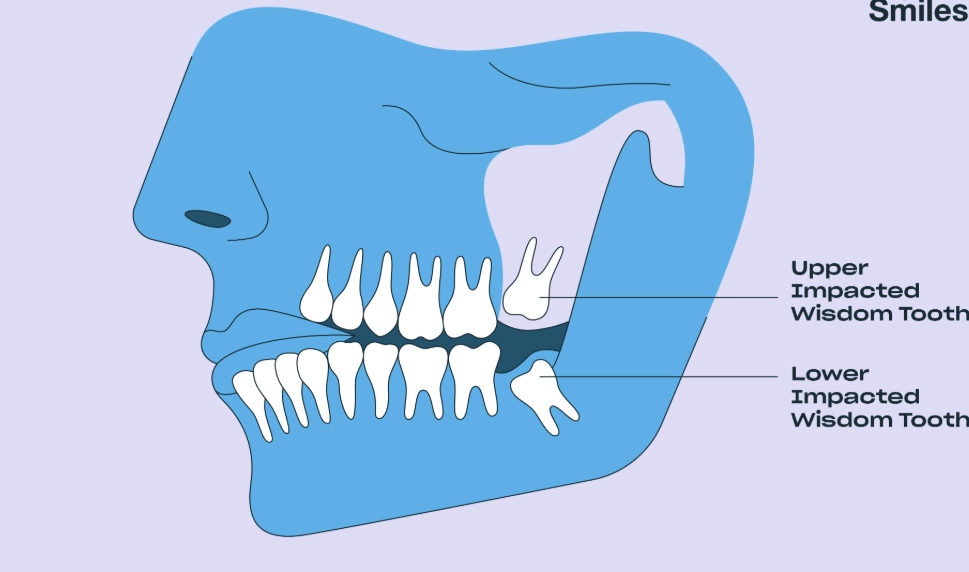
Forget horror stories. Most people are back to light activity in 2-3 days. Here's a day-by-day guide based on countless patient experiences.
Day 1-2: This is the peak. Plan to rest. You'll have gauze in your mouth to control bleeding (change it every 30-45 minutes). Swelling peaks around day 2-3—use ice packs (20 minutes on, 20 minutes off). Stick to a strict liquid/soft food diet: broths, yogurt, applesauce, protein shakes. Take your pain meds as prescribed, before the local anesthetic fully wears off.
Day 3-5: A turning point. Swelling and pain should start to subside. You can transition to slightly more substantial soft foods like mashed potatoes, scrambled eggs, and pasta. Begin gentle saltwater rinses (1/2 tsp salt in warm water) after 24 hours, but don't swish vigorously.
Day 7+: Stitches often dissolve or are removed. You can usually resume most normal eating, avoiding only very hard, crunchy, or spicy foods that can irritate the sockets. Most people return to work or school within a week.
Full healing of the bone underneath takes months, but you won't feel it. The biggest mistake I see? Patients feeling better on day 4 and deciding to eat chips or use a straw. The suction from a straw can dislodge the crucial blood clot, causing a painful dry socket. Just don't do it.
Your Top Wisdom Teeth Questions, Answered
 What's the one piece of advice you give everyone for recovery?
What's the one piece of advice you give everyone for recovery?The decision of when to remove your wisdom teeth isn't just a calendar check. It's a balance of preventative care and necessary intervention. Listen to your dentist's recommendations, but also look at your own X-rays. Ask questions: "What is this tooth likely to do in the next 5 years?" "What are the risks of waiting versus removing now?" Armed with the knowledge of the warning signs and a clear picture of the process, you can move forward with confidence, whether that means scheduling surgery or continuing with vigilant monitoring.