Let's cut straight to the point. The single most common question I get in my oral surgery practice isn't about pain or cost—it's about timing. "When is the best age for wisdom teeth removal?" Patients, often young adults and their parents, are looking for a clear answer. After over a decade of pulling thousands of these molars, the evidence and my experience point to a clear sweet spot: between the ages of 17 and 25. But that's just the headline. The real story is why this window exists, what happens if you're outside it, and how to navigate the decision for yourself or your teen.
This isn't about scaring you into surgery. It's about giving you the information you need to make a smart, proactive choice for your long-term oral health. Waiting until a toothache strikes at 2 AM is a strategy, but it's a terrible one.
In This Guide: What You'll Learn
The Science Behind the "Sweet Spot" Age (17-25)
Why is late adolescence to early adulthood the gold standard? It boils down to biology and predictability.
By age 17-18, the roots of the wisdom teeth are about one-half to two-thirds formed. This is the key. The roots haven't yet fully anchored themselves deep into your jawbone and wrapped around critical nerves (like the inferior alveolar nerve). Removing them at this stage is mechanically simpler. The bone surrounding them is also more elastic and forgiving in younger individuals. Healing is faster, with less post-operative swelling and discomfort.
Think of it like pulling a young sapling versus a mature tree. The sapling comes out with relative ease, leaving a smaller hole that fills in quickly. The mature tree has a vast, deep root system.
Furthermore, by this age, your oral surgeon can make a highly accurate prediction. Panoramic X-rays clearly show the teeth's position, angulation, and relationship to nerves. We can see if they're likely to become impacted (stuck), crowd other teeth, or erupt normally. The American Association of Oral and Maxillofacial Surgeons recommends an evaluation by age 18 for this exact reason. It's preventive care, not emergency care.
A Common Misconception I See: Many people think, "If my wisdom teeth aren't hurting, they're fine." This is the biggest mistake. Pain is a late-stage symptom. By the time a wisdom tooth hurts, it may have already caused a cavity in the adjacent molar, created a gum infection (pericoronitis), or started shifting your other teeth. Prevention is the whole point of timing it right.
A Decade-by-Decade Breakdown: From Teens to 40s+
Your experience with wisdom tooth extraction changes significantly with age. Here’s what you can realistically expect.
| Age Range | Typical Scenario & Why | Procedure & Recovery Notes |
|---|---|---|
| 17-21 | Proactive removal. Roots are partially formed, bone is less dense. Often recommended based on X-ray prediction of future problems (impaction, crowding). | Often straightforward. Faster healing (3-5 days for initial recovery). Lower risk of nerve-related complications. Many patients are still on parents' insurance. |
| 22-30 | The "catch-up" decade. Teeth may have partially erupted, leading to recurrent gum infections. Roots are fully formed, increasing complexity slightly. | Procedure can be more involved if teeth are impacted. Recovery might take 5-7 days to feel normal. Risk of dry socket is present but manageable. |
| 31-40+ | Problem-driven removal. Often due to pain, cysts, decay, or gum disease. Bone is denser, roots are fully developed and may be fused. | More likely to be a surgical extraction. Longer, potentially more uncomfortable recovery (7-10 days). Higher risk of complications like sinus communication (for upper teeth) or temporary nerve sensation changes. |
I had a patient, Mark, who came to me at 28. His lower left wisdom tooth had been "quiet" for years. Then, a dull ache started. The X-ray revealed it was horizontally impacted, slowly dissolving the roots of the molar in front of it. We saved the molar, but the extraction was tougher than it would have been a decade prior, and his recovery involved more jaw stiffness. His story is incredibly common.
What If You're Older Than 25? (It's Not Too Late!)
If you're reading this in your 30s, 40s, or beyond, don't panic. The goalposts move, but the game is still winnable. The calculus shifts from pure prevention to managing active or imminent problems. The surgery might be classified as more complex, but with modern techniques like minimally invasive surgery and piezoelectric ultrasonic bone surgery (which is gentler than drills), outcomes are excellent.
The conversation with your surgeon becomes more detailed. We'll spend more time discussing CT scans to map nerve pathways, the potential for bone grafting the socket to preserve jaw structure, and a meticulously planned recovery protocol.
What to Expect: Surgery Day & The Recovery Timeline
Knowing what's coming reduces anxiety immensely. Here’s a no-BS timeline.
The Day Before: Fill your prescriptions (pain meds, antibiotic if prescribed). Buy soft foods: yogurt, applesauce, mashed potatoes, protein shakes. Get a couple of extra ice packs. Set up a recovery nest with pillows, water, and entertainment.
Surgery Day (The First 24 Hours): You'll be under IV sedation or local anesthesia. You won't feel or remember a thing. The procedure itself takes about 45-90 minutes. You'll leave with gauze in your mouth and very numb. The key here is ice, rest, and liquid calories. Apply ice packs 20 minutes on, 20 minutes off. Sleep propped up. Don't use a straw—the suction can dislodge the blood clot.
Days 2-4 (The Swelling Peak): This is the toughest part. Swelling and stiffness peak around day 3. Bruising might appear. Transition to very soft foods. Start gentle saltwater rinses (no swishing, just let it dribble out) after 24 hours. Pain is manageable with medication. You'll be tired.
Days 5-7 (The Turnaround): Swelling and pain decrease significantly. You can often return to desk work or school. Start introducing slightly more solid foods like scrambled eggs or pasta. Stitches may dissolve or need removal.
Week 2+ (The Long Haul): Most people feel mostly normal. The sockets will slowly fill with tissue over the next few weeks. Avoid crunchy foods in the surgical areas. Full healing of the bone underneath takes months, but you won't feel it.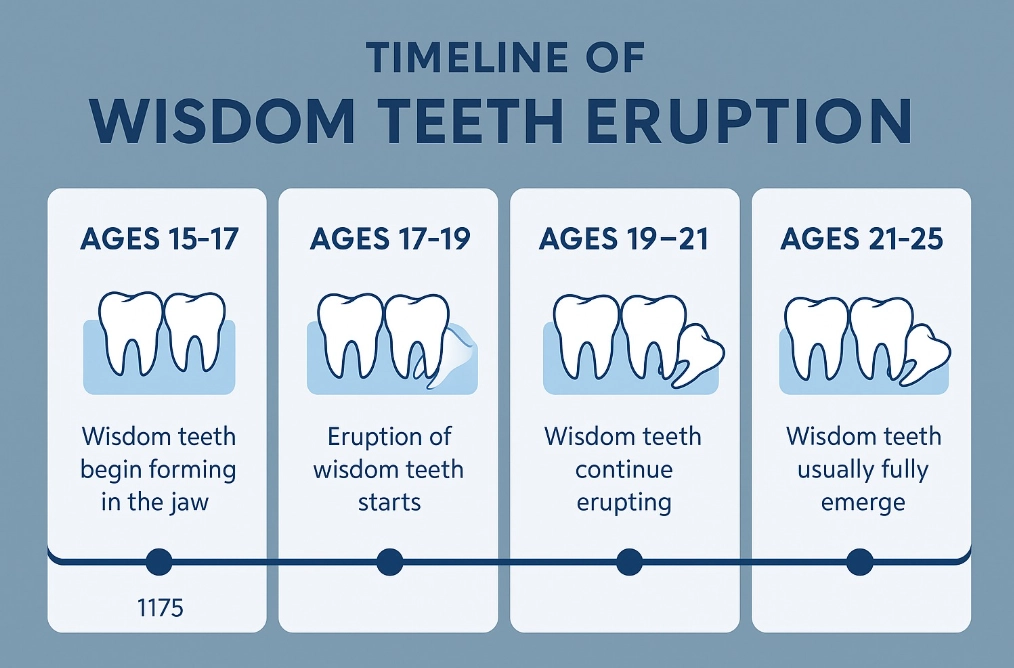
The Real Cost of Waiting Too Long
Beyond a more difficult surgery, delaying can lead to concrete, expensive problems:
- Damage to Adjacent Molars: Impacted wisdom teeth are notorious for causing cavities and bone loss on the side of your precious second molars. Fixing that can require a root canal, crown, or even loss of that tooth.
- Cyst Formation: A fluid-filled sac can develop around an impacted tooth, silently destroying jawbone. I've seen cases where this required significant bone grafting to repair.
- Orthodontic Relapse: If you spent years and thousands on braces, wisdom teeth can undo that work by causing crowding of your front teeth.
- Systemic Health Links: Chronic inflammation from partially erupted wisdom teeth (pericoronitis) is linked to broader health issues. The research, like studies referenced by the American Association of Oral and Maxillofacial Surgeons, shows potential connections to cardiovascular health.
Financially, an early, straightforward extraction is almost always cheaper than an emergency procedure plus the cost of fixing the damage it caused.
Your Top Questions, Answered
