Let's be honest, wisdom tooth pain is a special kind of misery. It's not just a toothache; it's a deep, throbbing ache in the back of your jaw that can ruin your day, your sleep, and your ability to enjoy a meal. You're not imagining it—it really is that disruptive. If you're reading this, you're probably in the thick of it, searching for relief that actually works. I've seen this scenario countless times in my practice. The good news? You don't have to just suffer through it. This guide cuts through the generic advice and gives you a clear, actionable plan based on what actually helps people get through this uncomfortable rite of passage.
In This Guide: Navigating Wisdom Tooth Pain
What Really Causes That Throbbing Pain?
It starts as a dull pressure, then graduates to a persistent ache. Why? Your wisdom teeth, or third molars, are the last to show up, usually between ages 17 and 25. There's often simply no room for them. Your jaw might be too small, or the teeth might come in at an angle. This isn't a design flaw, just an evolutionary leftover from when our ancestors needed the extra grinding power for a tougher diet.
The pain typically stems from a few key issues:
Pericoronitis: This is the big one. It means inflammation around the crown of a partially erupted tooth. A flap of gum tissue (called an operculum) can trap food and bacteria, creating a perfect pocket for infection. The pain is often sharp, localized, and may come with swelling and a bad taste.
Impaction: When the tooth is blocked from coming in fully—by other teeth, bone, or gum tissue—it's impacted. Pressure builds up, causing a deep, constant ache in your jawbone and potentially damaging the roots of neighboring molars.
Crowding and Pressure: Even if it's trying to come in straight, a wisdom tooth can push against its neighbors. You might feel a general soreness or pressure across your entire lower or upper jaw, and you might notice your other teeth feeling slightly shifted or tight.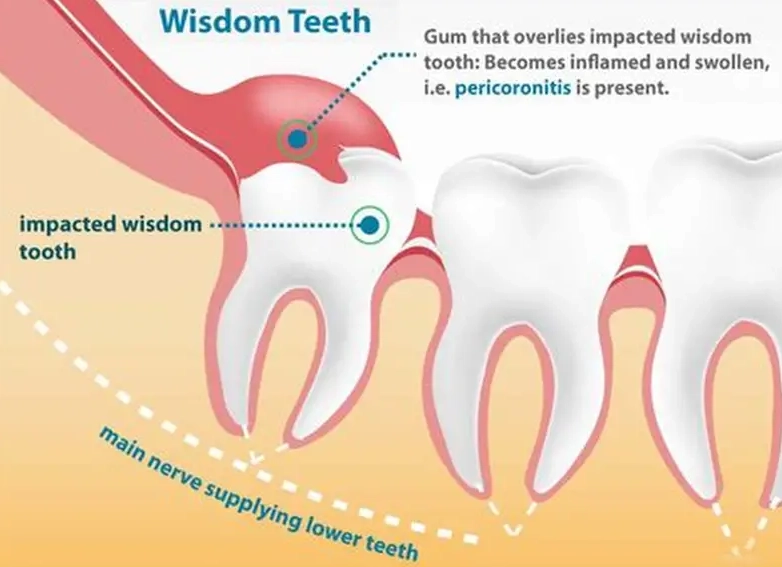
Your At-Home Pain Relief Toolkit (Before You See the Dentist)
You need relief now, not just a theory. Here’s a breakdown of what works, organized by what you likely have in your house or can get from a pharmacy.
Over-the-Counter Medications: The First Line of Defense
Don't just grab any painkiller. For dental inflammation, you need a strategic approach. Ibuprofen (Advil, Motrin) is typically more effective than acetaminophen (Tylenol) for this type of pain because it directly reduces inflammation. A common and effective regimen is alternating ibuprofen and acetaminophen every 3-4 hours (after checking with your doctor or pharmacist for any contraindications for you). This targets pain through two different pathways.
Important: Always follow package directions. Don't exceed the daily dose, and take them with food to protect your stomach.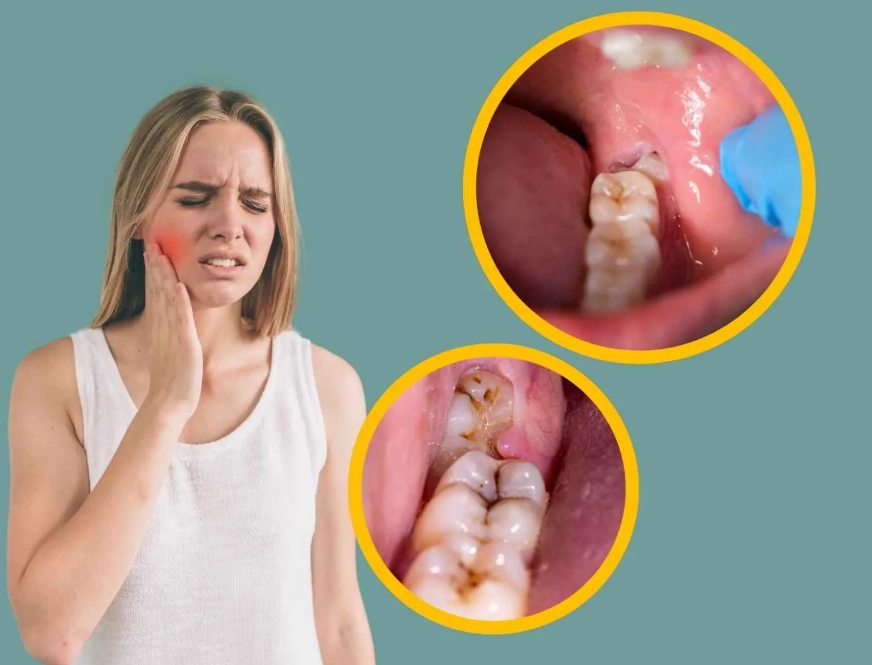
Salt Water Rinse: The Underestimated Powerhouse
This isn't just old-fashioned advice; it's clinically sound. A warm salt water rinse (1/2 teaspoon of salt in a cup of warm water) is mildly antiseptic and helps draw out fluid from inflamed tissues, reducing swelling. Gently swish it around the affected area for 30 seconds after meals and before bed. It's simple, safe, and surprisingly effective for cleaning out trapped debris and soothing irritated gums.
Cold Therapy vs. Warm Compress: Knowing Which to Use
This is where people get it wrong. If the area is visibly swollen, puffy, or feels hot to the touch, use a cold compress. Wrap an ice pack or a bag of frozen peas in a thin cloth and apply it to the outside of your cheek for 15 minutes on, 15 minutes off. This constricts blood vessels, reduces swelling, and numbs the pain.
If the pain is a deep, muscular ache in your jaw with no significant external swelling, a warm, moist compress against your jaw can help relax the tense muscles and improve blood flow. Use a warm (not hot) washcloth.
Avoid putting aspirin directly on the gum. It can cause a chemical burn and won't help the underlying issue.
Red Flags: When Home Care Isn't Enough
You can manage mild discomfort at home, but certain symptoms are your body's way of shouting for professional help. Ignoring these can turn a manageable problem into a serious infection or cause permanent damage.
| Symptom | What It Might Mean | Action Required |
|---|---|---|
| Severe, unrelenting pain that OTC meds don't touch | Advanced infection or abscess forming. | Call your dentist immediately. |
| Visible swelling in your cheek, jaw, or gums that's getting worse | Spreading infection (cellulitis). | Dentist or emergency room if you can't breathe/swallow. |
| Fever, chills, or general malaise | Your body is fighting a systemic infection. | Contact your dentist or doctor same day. |
| Difficulty opening your mouth (trismus) or swallowing | Inflammation affecting jaw muscles or throat. | Urgent dental care needed. |
| Pus oozing from around the tooth | Clear sign of an active abscess. | Requires professional drainage and antibiotics. |
| Pain radiating to your ear, temple, or neck | Referred pain from nerve involvement. | Schedule a dental evaluation promptly. |
The Road to Extraction and Recovery
If your dentist recommends removal—and for problematic wisdom teeth, it's often the only permanent solution—knowing what to expect can ease a lot of anxiety. The procedure itself is usually done under local anesthesia, sometimes with sedation if you're anxious or if all four are being removed at once.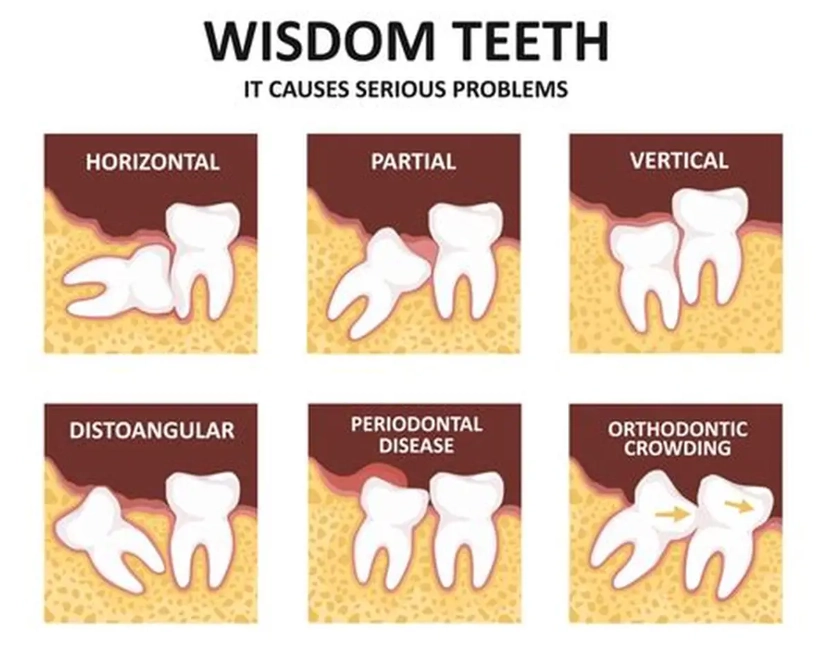
The First 24-48 Hours Are Critical: Your dentist will give you specific instructions, but the universal goals are to control bleeding, minimize swelling, and prevent a painful complication called a dry socket.
Bleeding: Bite down firmly on the gauze pad placed over the extraction site for 30-60 minutes. Change it as directed. Some oozing is normal for the first day.
Swelling: This peaks around 48 hours post-op. Use an ice pack on the outside of your cheek consistently for the first day (20 minutes on, 20 minutes off).
Dry Socket: This happens if the blood clot that forms in the socket gets dislodged too early, exposing bone and nerves. It's excruciating. To prevent it: Do not use straws, spit forcefully, or smoke for at least a week. These actions create suction that can pull the clot out. Stick to soft, cool foods like yogurt, applesauce, and mashed potatoes initially.
Pain Management Post-Op: Your dentist will likely prescribe pain medication or reinforce the OTC regimen. Start taking it before the local anesthesia fully wears off to stay ahead of the pain. A common mistake is waiting until you're in agony to take the first dose.
Healing is a process. Full bone remodeling takes months, but the significant discomfort usually subsides within 3-7 days. Follow-up with your dentist if pain suddenly worsens after a few days (a sign of dry socket) or if you develop a fever.
Your Top Wisdom Tooth Pain Questions Answered
My wisdom tooth pain comes and goes. Can I just manage it forever with painkillers?
That's a risky strategy. Intermittent pain often indicates chronic pericoronitis—repeated cycles of mild infection and inflammation. Each episode can cause a little more damage to the surrounding bone and gum. Long-term, this can weaken the support for the tooth in front of it, potentially leading to its loss. Painkillers mask the symptom but don't address the underlying, progressive problem.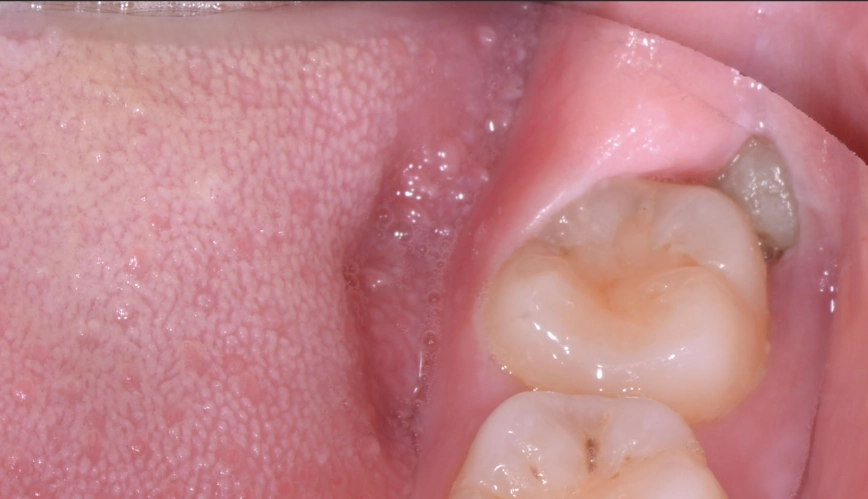
Is it normal for wisdom tooth pain to cause headaches and earaches?
Unfortunately, yes, it's very common. The nerves that supply your lower teeth and jaw are closely linked to those that supply sensation to parts of your ear, temple, and neck. Inflammation and pressure from an impacted or infected wisdom tooth can easily cause referred pain in these areas. If you're getting recurring headaches or earaches with no other clear cause, your back teeth deserve a close look.
I'm terrified of the extraction. Is it as bad as people say?
The fear is almost always worse than the reality, especially with modern dentistry. The procedure itself is painless due to effective anesthesia. The recovery can be uncomfortable, but it's manageable with the right plan (ice, medication, soft foods). Compare 3-5 days of managed post-op discomfort to years of recurring pain, infections, and the risk of damaging other teeth. For a truly problematic tooth, extraction is the shorter, simpler path to long-term relief. Discuss sedation options with your dentist if anxiety is the main barrier.
Can a wisdom tooth cause pain on the opposite side of my jaw?
It's less common, but possible. This is usually due to a change in your bite. If one side is painful, you might unconsciously start chewing only on the other side. This overworks the muscles and joints on the "good" side, leading to muscular pain, fatigue, and even temporomandibular joint (TMJ) discomfort. So while the source is the painful wisdom tooth, the symptom can manifest elsewhere.
What's the one thing most people forget to do that makes recovery harder?
Staying hydrated. After surgery, you're on soft foods and maybe taking pain meds that can cause constipation. Dehydration makes everything worse—headaches, fatigue, and can even slow healing. Sip water constantly. Avoid dehydration and keep your body's recovery systems running smoothly. It sounds simple, but it's the most frequently neglected part of post-op care.